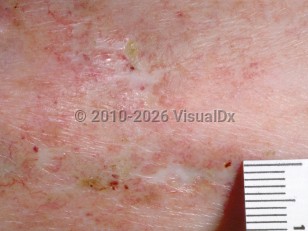
Livedoid vasculopathy
Alerts and Notices
Important News & Links
Synopsis

Livedoid vasculopathy (LV), also known as livedoid vasculitis, presents with retiform purpura or ulcers on the lower legs that may progress to atrophie blanche (AB). LV is caused by vaso-occlusion of the cutaneous microcirculation that manifests histopathologically as hyalinization of vessels leading to fibrin thrombi. LV is a rare condition, with an estimated incidence of 1:100 000 per year and an increased incidence during summer months and during pregnancy. It tends to affect young to middle-aged adults, with a median age of onset of 30-50 years, and has a female-to-male ratio of 2-3:1.
The pathogenesis of LV is not well understood, but it is likely related to increased coagulability and/or decreased fibrinolysis. The strongest risk factor is a hypercoagulable state with laboratory evaluation positive for a known cause of thrombophilia in 40%-50% of patients in retrospective cohort studies. The second most common risk factor is connective tissue disease. LV can also be associated with monocolonal gammopathy, with hepatitis B or C, or can be idiopathic.
LV follows a chronic time course, with lesions often developing for months before a definitive diagnosis is made. In a recent case series, the median interval between symptom onset and diagnosis was 10 months and between onset and treatment was 22.5 months.
The condition is rare in children.
The pathogenesis of LV is not well understood, but it is likely related to increased coagulability and/or decreased fibrinolysis. The strongest risk factor is a hypercoagulable state with laboratory evaluation positive for a known cause of thrombophilia in 40%-50% of patients in retrospective cohort studies. The second most common risk factor is connective tissue disease. LV can also be associated with monocolonal gammopathy, with hepatitis B or C, or can be idiopathic.
LV follows a chronic time course, with lesions often developing for months before a definitive diagnosis is made. In a recent case series, the median interval between symptom onset and diagnosis was 10 months and between onset and treatment was 22.5 months.
The condition is rare in children.
Codes
ICD10CM:
L95.0 – Livedoid vasculitis
SNOMEDCT:
53312001 – Vasculitis of the skin
L95.0 – Livedoid vasculitis
SNOMEDCT:
53312001 – Vasculitis of the skin
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:06/03/2020
Last Updated:06/04/2020
Last Updated:06/04/2020
Livedoid vasculopathy