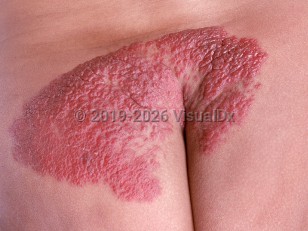
Lumbosacral skin lesion
Alerts and Notices
Important News & Links
Synopsis

Congenital lumbosacral cutaneous lesions along the paraspinal region can often be a marker of occult spinal dysraphism, a failure of one or more components of the spinal cord or canal to fuse properly during development. It is thought that about 75% of occult spinal dysraphism cases are associated with a congenital cutaneous lesion, often at the midline lumbosacral region. Women are more often affected than men. If spinal dysraphism is present, the spinal cord can be tethered as the child grows, and spinal nerve function can be compromised. Early testing, diagnosis, and treatment are necessary.
Such lesions can take various forms, including lipomas, dermal sinuses, tails, deviated gluteal clefts, hemangiomas, hamartomas, dimples, or pigmentary changes. However, these lesions can also occur in isolation of any neurologic defect; depending on the level of risk for occult spinal dysraphism associated with the particular lesion or lesions, radiographic investigation with MRI or ultrasound may be warranted. Early detection and treatment of spinal cord anomalies is important to prevent tethering of the spinal cord and neurological deficits later in life.
The highest risk for occult spinal dysraphism occurs in the presence of two or more congenital lumbosacral midline cutaneous lesions of any kind. Any one lesion in the presence of spinal cord dysfunction is also considered high risk. Lipomas, tails, aplasia cutis congenita, dermal sinuses, dermoid cysts, and large infantile hemangiomas (≥ 2.5 cm) are all independently considered high risk for occult spinal dysraphism. All high-risk lesions require MRI evaluation for spinal anomalies.
Moderate-risk lesions include atypical dimples, smaller hemangiomas, deviated gluteal folds, and hypertrichosis (including faun tail or silky down). Moderate risk lesions also require MRI evaluation, although ultrasound can be completed first if the child is younger than 6 months of age as the vertebral bodies have not yet ossified.
Low-risk lesions that do not necessitate further imaging include simple dimples, port-wine stains, pigmented nevi, and congenital dermal melanocytosis.
Related topic: Spina bifida
Such lesions can take various forms, including lipomas, dermal sinuses, tails, deviated gluteal clefts, hemangiomas, hamartomas, dimples, or pigmentary changes. However, these lesions can also occur in isolation of any neurologic defect; depending on the level of risk for occult spinal dysraphism associated with the particular lesion or lesions, radiographic investigation with MRI or ultrasound may be warranted. Early detection and treatment of spinal cord anomalies is important to prevent tethering of the spinal cord and neurological deficits later in life.
The highest risk for occult spinal dysraphism occurs in the presence of two or more congenital lumbosacral midline cutaneous lesions of any kind. Any one lesion in the presence of spinal cord dysfunction is also considered high risk. Lipomas, tails, aplasia cutis congenita, dermal sinuses, dermoid cysts, and large infantile hemangiomas (≥ 2.5 cm) are all independently considered high risk for occult spinal dysraphism. All high-risk lesions require MRI evaluation for spinal anomalies.
Moderate-risk lesions include atypical dimples, smaller hemangiomas, deviated gluteal folds, and hypertrichosis (including faun tail or silky down). Moderate risk lesions also require MRI evaluation, although ultrasound can be completed first if the child is younger than 6 months of age as the vertebral bodies have not yet ossified.
Low-risk lesions that do not necessitate further imaging include simple dimples, port-wine stains, pigmented nevi, and congenital dermal melanocytosis.
Related topic: Spina bifida
Codes
ICD10CM:
Q82.8 – Other specified congenital malformations of skin
SNOMEDCT:
403559003 – Cutaneous lesion resulting from spinal dysraphism
Q82.8 – Other specified congenital malformations of skin
SNOMEDCT:
403559003 – Cutaneous lesion resulting from spinal dysraphism
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/11/2019
Last Updated:09/15/2019
Last Updated:09/15/2019
Lumbosacral skin lesion