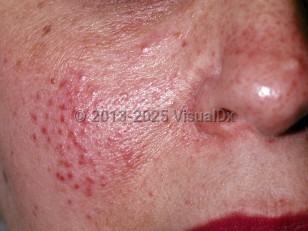
Lupus miliaris disseminatus faciei - External and Internal Eye
See also in: OverviewAlerts and Notices
Important News & Links
Synopsis

Lupus miliaris disseminatus faciei (LMDF), also known as acne agminata and acnitis, is a relatively rare papular eruption of the face. Because of its characteristic granulomatous histology, LMDF was previously thought to be a variant of cutaneous tuberculosis, granulomatous rosacea, or sarcoidosis. However, today many consider it to be a distinct entity. Some authors have proposed use of the term facial idiopathic granulomas with regressive evolution (acronym FIGURE); however, this term has not been widely accepted.
The exact etiology of LMDF is unknown, but the current hypotheses include an inflammatory reaction to pilosebaceous units, injured hair follicles, or Cutibacterium acnes (formerly Propionibacterium acnes). It is also proposed that the activation of the IL-23 / IL-17 axis might be involved in the disease pathogenesis.
LMDF typically affects adolescents and adults of both sexes, although childhood cases and cases in elderly patients have also been reported. Lesions are usually asymptomatic and resolve spontaneously in 1-3 years with pitted scars. The eruption does not have known associations with any systemic diseases.
The exact etiology of LMDF is unknown, but the current hypotheses include an inflammatory reaction to pilosebaceous units, injured hair follicles, or Cutibacterium acnes (formerly Propionibacterium acnes). It is also proposed that the activation of the IL-23 / IL-17 axis might be involved in the disease pathogenesis.
LMDF typically affects adolescents and adults of both sexes, although childhood cases and cases in elderly patients have also been reported. Lesions are usually asymptomatic and resolve spontaneously in 1-3 years with pitted scars. The eruption does not have known associations with any systemic diseases.
Codes
ICD10CM:
L93.2 – Other local lupus erythematosus
SNOMEDCT:
397845003 – Granulomatous rosacea
L93.2 – Other local lupus erythematosus
SNOMEDCT:
397845003 – Granulomatous rosacea
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/10/2020
Last Updated:05/10/2020
Last Updated:05/10/2020
Lupus miliaris disseminatus faciei - External and Internal Eye
See also in: Overview