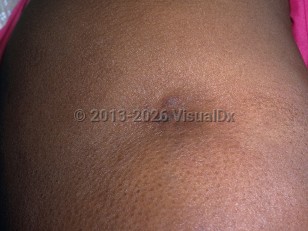
Lupus panniculitis in Adult
Alerts and Notices
Important News & Links
Synopsis

Lupus panniculitis, also known as lupus profundus, is considered a rare subtype (2%-3%) of chronic cutaneous lupus erythematosus, with tender, indurated, subcutaneous nodules or plaques located most frequently on the face, proximal extremities, breasts, and buttocks, with or without overlying cutaneous changes.
Lupus panniculitis can be associated with overlying discoid lupus erythematosus (DLE) in approximately one-third of individuals. Lupus panniculitis is thought to be caused by an autoimmune reaction in the deep dermis and adipose tissue. The first stage of lupus panniculitis is active inflammation with painful nodules, followed by the second stage of subcutaneous atrophy, which can be cosmetically disfiguring.
Lupus panniculitis, like systemic lupus erythematosus (SLE), occurs more commonly in women. Lupus panniculitis develops in approximately 5% of patients with SLE but can occur as an isolated disease. Cutaneous manifestations of lupus panniculitis can develop years before or after the diagnosis of SLE. The average age of onset is 30-40 years.
Male sex, lower extremity involvement, and concomitant DLE are associated with SLE.
Lupus panniculitis can be associated with overlying discoid lupus erythematosus (DLE) in approximately one-third of individuals. Lupus panniculitis is thought to be caused by an autoimmune reaction in the deep dermis and adipose tissue. The first stage of lupus panniculitis is active inflammation with painful nodules, followed by the second stage of subcutaneous atrophy, which can be cosmetically disfiguring.
Lupus panniculitis, like systemic lupus erythematosus (SLE), occurs more commonly in women. Lupus panniculitis develops in approximately 5% of patients with SLE but can occur as an isolated disease. Cutaneous manifestations of lupus panniculitis can develop years before or after the diagnosis of SLE. The average age of onset is 30-40 years.
Male sex, lower extremity involvement, and concomitant DLE are associated with SLE.
Codes
ICD10CM:
L93.2 – Other local lupus erythematosus
SNOMEDCT:
239888002 – Lupus panniculitis
L93.2 – Other local lupus erythematosus
SNOMEDCT:
239888002 – Lupus panniculitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/26/2025
Last Updated:06/01/2025
Last Updated:06/01/2025
Lupus panniculitis in Adult