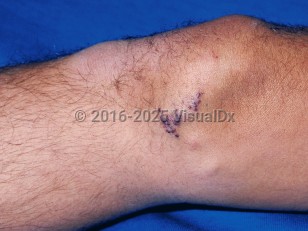
Lymphangioma circumscriptum in Child
See also in: AnogenitalAlerts and Notices
Important News & Links
Synopsis

Lymphatic malformations (LMs) consist of vesicles or cysts filled with lymphatic fluid. Macrocystic LMs, formerly known as cystic hygroma, are larger than 1 cm in diameter. Microcystic LM, formerly known as lymphangioma circumscriptum, lymphangioma simplex, verrucous hemangioma, and angiokeratoma circumscriptum, is a benign congenital disorder that consists of dilated superficial lymphatic channels or large cysts filled with lymphatic fluid.
Microcystic LMs occur as a result of an error in the morphogenesis of the lymphatic vessels, leading to a disorder of lymph drainage. However, the exact etiology of this error is unknown. Subcutaneous lymphatic cisterns communicate through dilated channels with the skin's surface to form localized clusters of translucent vesicles that contain clear or serosanguineous lymphatic fluid. Unlike venous malformations, microcystic LMs do not swell with the Valsalva maneuver but rather swell periodically, often in association with viral illnesses. Microcystic LMs form in utero and are, thus, present at birth or become more apparent early in childhood. Most are diagnosed before the age of 2 years. At times, these lesions are not detected until complications arise, such as infection or bleeding. Microcystic LMs can occur as combined lymphatic and vascular malformations. These combined lesions are more commonly seen in the head region and can interfere with normal development of the jaw.
The presentation of microcystic LMs can vary greatly, usually depending on the site and depth. Distribution of microcystic LMs is most commonly on the face, although they may occur on the proximal extremities, groin, axilla, or oral (oral lymphangioma) or genital areas. Lesions tend to grow proportionally and enlarge with age, which may delay the diagnosis. These lesions may intermittently leak lymphatic fluid, and they can bleed and become purple or nodular.
Microcystic LMs have a propensity to the face, especially in the mandibular area, and may cause facial asymmetry. Sepsis is a serious complication that may occur in lesions close to the alimentary tract such as the face and pelvis. Other locations that can cause extracutaneous complications include intraorbital LM, which can cause exophthalmia and ocular dystopia, or LM on the tongue, which can impair speech and produce halitosis.
Intervention is typically not necessary unless lesions are symptomatic. The most common symptoms include pain, inflammatory flares, minor bleeding, and recurrent episodes of cellulitis. Historically, surgical treatment was the treatment of choice for microcystic LM, although recurrence was frequent and surgical morbidity was considerable, as the entire lesions needed to be excised. Newer therapies, including the use of sclerosing agents, have shown promising long-term results.
Microcystic LMs occur as a result of an error in the morphogenesis of the lymphatic vessels, leading to a disorder of lymph drainage. However, the exact etiology of this error is unknown. Subcutaneous lymphatic cisterns communicate through dilated channels with the skin's surface to form localized clusters of translucent vesicles that contain clear or serosanguineous lymphatic fluid. Unlike venous malformations, microcystic LMs do not swell with the Valsalva maneuver but rather swell periodically, often in association with viral illnesses. Microcystic LMs form in utero and are, thus, present at birth or become more apparent early in childhood. Most are diagnosed before the age of 2 years. At times, these lesions are not detected until complications arise, such as infection or bleeding. Microcystic LMs can occur as combined lymphatic and vascular malformations. These combined lesions are more commonly seen in the head region and can interfere with normal development of the jaw.
The presentation of microcystic LMs can vary greatly, usually depending on the site and depth. Distribution of microcystic LMs is most commonly on the face, although they may occur on the proximal extremities, groin, axilla, or oral (oral lymphangioma) or genital areas. Lesions tend to grow proportionally and enlarge with age, which may delay the diagnosis. These lesions may intermittently leak lymphatic fluid, and they can bleed and become purple or nodular.
Microcystic LMs have a propensity to the face, especially in the mandibular area, and may cause facial asymmetry. Sepsis is a serious complication that may occur in lesions close to the alimentary tract such as the face and pelvis. Other locations that can cause extracutaneous complications include intraorbital LM, which can cause exophthalmia and ocular dystopia, or LM on the tongue, which can impair speech and produce halitosis.
Intervention is typically not necessary unless lesions are symptomatic. The most common symptoms include pain, inflammatory flares, minor bleeding, and recurrent episodes of cellulitis. Historically, surgical treatment was the treatment of choice for microcystic LM, although recurrence was frequent and surgical morbidity was considerable, as the entire lesions needed to be excised. Newer therapies, including the use of sclerosing agents, have shown promising long-term results.
Codes
ICD10CM:
D18.01 – Hemangioma of skin and subcutaneous tissue
SNOMEDCT:
238799002 – Lymphangioma circumscriptum
D18.01 – Hemangioma of skin and subcutaneous tissue
SNOMEDCT:
238799002 – Lymphangioma circumscriptum
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:03/09/2020
Lymphangioma circumscriptum in Child
See also in: Anogenital