Normally, most of the interstitial fluid is reabsorbed via the venous microcirculation and returns to systemic circulation. The remainder (approximately 10%) has a relatively high protein concentration and is drained by blind-ended lymphatic capillaries. Once the protein-rich interstitial fluid enters the lymphatic system, it is referred to as lymph. Impaired lymphatic drainage causes buildup of lymph in the interstitial spaces, leading to tissue swelling.
It has been reported that lymphedema affects as many as 200 million people worldwide and approximately 3 million people in the United States. Lymphedema affects females more often than males.
Lymphedema may be primary, referring to a developmental abnormality of the lymphatic system, or secondary (acquired). Primary lymphedema is rare, affecting approximately 1 in 100 000 children. It may rarely be associated with other syndromes such as Turner syndrome, Noonan syndrome, and yellow nail syndrome.
Based on the age of onset, primary lymphedema can be subdivided into 3 categories: congenital lymphedema (presenting at or shortly after birth), lymphedema praecox (occurring around puberty or shortly thereafter), and lymphedema tarda (starting late in life). Lymphedema praecox is the most common type of primary lymphedema.
Secondary, or acquired, lymphedema is much more common. It results from damage or obstruction of previously normal lymphatics. Filariasis is the most common cause of secondary lymphedema worldwide. Treatment related to cancer is the most common cause of secondary lymphedema in the United States. Major risk factors include axillary lymph node dissection and adjuvant radiation therapy. Other causes include destruction by surgery, radiation, or infection. Secondary lymphedema is typically diagnosed in patients aged 50-58 years.
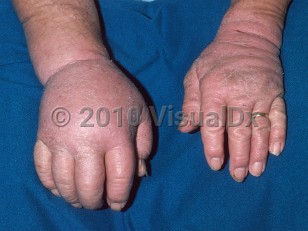
Lymphedema is a clinical diagnosis. The lower extremities are the most common location. Lymphedema can be unilateral or bilateral. Early-stage lymphedema mimics venous edema (transient pitting edema). Chronic lymphedema is characterized by skin thickening and tissue fibrosis.
Clinical Staging of Lymphedema:
Based on clinical findings in a physical examination, the International Society of Lymphology (ISL) developed a staging system that divides lymphedema into 4 stages:
- Stage 0 (subclinical) – Swelling is not evident. Heaviness and discomfort.
- Stage 1 (spontaneously reversible) – Swelling relieved by limb elevation. Includes pitting edema.
- Stage 2 (spontaneously irreversible) – Swelling not improved by limb elevation. May or may not include pitting edema.
- Stage 3 (lymphostatic elephantiasis) – Swelling not improved by limb elevation. Skin hardening, nonpitting edema, verrucous changes, and recurrent soft tissue infections.