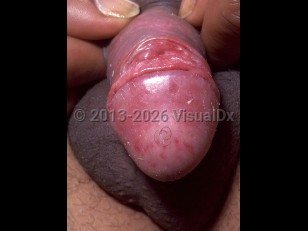
Male genital candidiasis - Anogenital in
Alerts and Notices
Important News & Links
Synopsis

In its mildest form, the condition may be intermittent and transient. Candida most often infects warm, moist, occluded areas, and the proximal shaft of the penis, the scrotum, and the crural folds are frequently involved. Candidal balanitis is an infection of the glans penis. It occurs more frequently in uncircumcised males. Genital and crural candidiasis can be accompanied by burning and pruritus.
Immunocompromised populations are at an increased risk of developing candidiasis. These patients include those with diabetes, HIV, systemic lupus erythematosus (SLE), and obesity, and patients being treated with corticosteroids or chemotherapy. Many patients will first present with candidal infections while the underlying cause of their immunocompromised state remains unknown; therefore, it is imperative that the physician keep these causes in mind. Recent oral antibiotic therapy is a further predisposing factor.
Diabetes is recognized as a risk factor for candidal infections because of decreased vascularity and the increase in blood glucose, which provides the best growth media for Candida. Candidal infections are one of the first presenting signs of previously undetected diabetes. Excellent glucose control will decrease the rates of candidiasis.
Patients with HIV infection may first present with mucocutaneous candidal infections or genital candidiasis. High suspicion should be held for patients who have recurrent candidal infections along with other risk factors for the contraction of the virus. Early detection of HIV holds importance for patient management as well as containing the spread of the virus.
Patients with autoimmune conditions like SLE, rheumatoid arthritis, scleroderma, Goodpasture syndrome, and granulomatosis with polyangiitis who are being treated with corticosteroids are at an increased risk for candidal infections. As these patients are being treated with high levels of immunosuppressives, it is important to look for mucocutaneous and genital candidiasis.
Related topic: oral candidiasis
Codes
B37.42 – Candidal balanitis
SNOMEDCT:
240708000 – Penile candidiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/22/2021
 Patient Information for Male genital candidiasis - Anogenital in
Patient Information for Male genital candidiasis - Anogenital in - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient