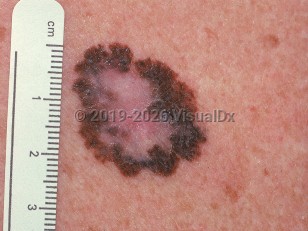
Melanoma in Adult
See also in: Anogenital,Hair and Scalp,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

The etiology of melanoma is incompletely understood, although ultraviolet radiation is believed to play a role in some melanomas and knowledge of the melanoma genome continues to advance. Melanoma susceptibility genes have been associated with melanoma tumor syndromes and some other familial tumor syndromes; these include mutations in CDKN2A/CDK4 (familial atypical multiple mole melanoma syndrome [FAMMM syndrome]), BAP1 (BAP1 cancer syndrome), MITF (MITF tumor syndrome), TERT/Shelterin complex, and PTEN). Melanoma has been shown to have one of the highest mutation rates of any cancer type, reflective of its clinical and pathologic diversity and resistance to treatment in advanced stages.
Risk factors for melanoma include a family history or prior personal history of melanoma, a history of severe or blistering sunburns, a changing mole, a giant congenital nevus (greater than 20 cm), older age, lighter skin phototype, and multiple atypical nevi. In a case control study of over 1000 patients, 3 or more iris pigmented lesions conferred an increased risk for cutaneous melanoma. Men are more prone to developing melanoma on the head, neck, and trunk, whereas women tend to develop melanoma on the arms and legs. Parkinson disease is associated with an increased risk of melanoma. The median age at diagnosis is in the 60s. The number of new cases of melanoma in the United States has been steadily rising since 1975, with an estimated 76 380 new cases of melanoma in the United States in 2016. The lifetime risk of being diagnosed with melanoma in the United States is estimated to be 2.1%.
The primary prognostic feature of melanoma is the depth of invasion, which is measured histologically in millimeters and referred to as the Breslow thickness. Early diagnosis and treatment of thin melanomas can lead to a generally favorable prognosis (97% and 93% for 5- and 10-year survival for a T1aN0M0 melanoma; see staging below), while with advanced forms the prognostic outlook is less favorable. Mortality rates are higher among men than among women. Melanoma can metastasize to any organ of the body. The most frequent sites are skin / subcutaneous, lymph nodes, lungs, liver, and brain. Rarely, primary diffuse meningeal melanomatosis can occur.
Related topic: amelanotic melanoma
Codes
C43.9 – Malignant melanoma of skin, unspecified
SNOMEDCT:
372244006 – Malignant melanoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:05/31/2023
 Patient Information for Melanoma in Adult
Patient Information for Melanoma in Adult- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient