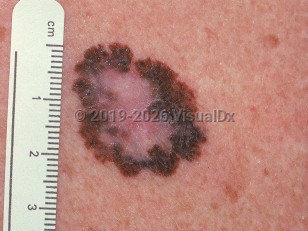
Melanoma - Anogenital in
See also in: Overview,Hair and Scalp,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Melanomas can be found anywhere on the body, including the glans penis, foreskin, shaft, anus (see anorectal melanoma), urethra, and the scrotum. Primary melanomas of the glans penis and male urethra are rare, representing < 0.1% of all melanomas. Anogenital melanoma is responsible for approximately 0.05% of all colorectal malignancies and 1% of all anal canal cancers. Scrotal melanomas are equally as rare. Melanomas of the genitalia most often arise de novo in elderly individuals.
The best prognostic indicator is the Breslow thickness, a measure of the depth of invasion of the melanoma. Lesions less than 0.75 mm in thickness generally have a good prognosis, while lesions greater than 3.5 mm have a very poor prognosis. A higher percentage of male genitourinary melanomas than cutaneous melanomas are at an advanced stage at the time of diagnosis, either as a result of late presentation (urethral melanoma) or delay in seeking medical care, leading to a poorer outcome. Urethral melanomas, especially, have a worse prognosis than cutaneous melanoma.
There are no established guidelines for staging of mucosal melanoma and scrotal melanoma. For glans and penile melanoma, both the American Joint Committee on Cancer (AJCC) staging criteria and a 3-stage system have been used:
Stage 1: Lesion is confined to the penis.
Stage 2: Metastatic to the regional lymph nodes.
Stage 3: Disseminated disease.
Codes
C43.9 – Malignant melanoma of skin, unspecified
SNOMEDCT:
372244006 – Malignant melanoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/14/2022
 Patient Information for Melanoma - Anogenital in
Patient Information for Melanoma - Anogenital in - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient