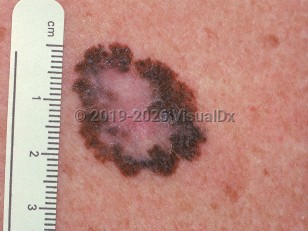
Melanoma - Oral Mucosal Lesion
See also in: Overview,Anogenital,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Melanoma is a rare malignancy of the oral cavity. It accounts for around 0.5% of all melanomas. Black individuals and individuals of Japanese descent are affected more often. There is a 2:1 male predilection, and most occur in the sixth decade of life or later.
Oral melanoma can present as a painless, bleeding mass or ulcer of the hard palate or maxillary gingiva, but about 60% of cases are asymptomatic and identified incidentally during a dental examination. It tends to be diagnosed when advanced, and only approximately one-third of patients give a history of a pre-existing pigmented lesion, either nevus or mucosal melanosis. The risk factors for oral melanoma are not well studied. Smoking, irritation from dentures, and alcohol use have been proposed but not confirmed as risk factors. Only around 10%-38% of patients survive 5 years or more.
Related topic: nail melanoma
Codes
C43.9 – Malignant melanoma of skin, unspecified
SNOMEDCT:
372244006 – Malignant melanoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:01/27/2022
 Patient Information for Melanoma - Oral Mucosal Lesion
Patient Information for Melanoma - Oral Mucosal Lesion- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient