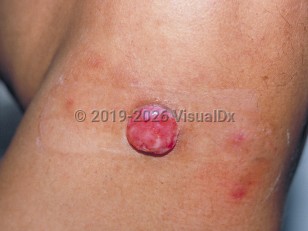
Merkel cell carcinoma
Alerts and Notices
Important News & Links
Synopsis

MCC favors older adults, with a median age of 75-80 years at the time of diagnosis. It is more common among individuals of Northern European descent than those of African, Asian, or Hispanic descent. MCC is also more common in immunocompromised individuals. Two important etiologic factors for MCC are the Merkel cell polyomavirus (MCPyV) and ultraviolet (UV) exposure. Patients with MCC who are polyomavirus negative have more aggressive tumors.
MCC typically presents as an asymptomatic, firm, nontender, solitary, rapidly growing nodule. It occurs most frequently on the head and neck but can also be seen elsewhere on the body.
A high index of suspicion is needed for diagnosis. In one study, the most frequent prebiopsy diagnosis rendered was of a benign lesion, such as an acneiform lesion or cyst.
Despite aggressive treatment, recurrence rates are high, metastases are common, and 5-year relative survival is approximately 60% in the United States based on data from a national database from 2005-2014. The recurrence rate of MCC has been estimated to be approximately 40%, and the majority (90%) have been observed within the first 3 years. Factors associated with an increased risk of recurrence include higher pathologic stage, immunosuppression, male sex, older age, and a known primary lesion in patients with clinically detectable nodal disease. Survival rates were higher in women (68%), lower in non-Hispanic Black individuals (54%), and decreased with later stage, number of lymph nodes involved, and older age at diagnosis, as well as with the involvement of certain locations such as the trunk.
MCC, as with other neuroendocrine tumors, has been associated with rare paraneoplastic neurologic syndromes, and patients may present with neurologic symptoms such as ataxia, weakness, and confusion.
Codes
C4A.9 – Merkel cell carcinoma, unspecified
SNOMEDCT:
253001006 – Merkel cell carcinoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/29/2022