Mucormycosis can cause serious life-threatening infections in compromised hosts. While rhinocerebral mucormycosis is the most common form of the disease, mucormycosis can involve the skin, pulmonary, renal, and gastrointestinal organs, or it can disseminate. The underlying risk factor can influence the clinical manifestation; rhinocerebral disease is common in people with diabetes, whereas patients with hematological malignancies or neutropenia usually have sinus and/or pulmonary disease and, more rarely, gastrointestinal disease. Although uncommon, in renal transplant patients, the primary location of infection when it does happen remains rhinocerebral and pulmonary, but up to 10% can involve the transplanted renal allograft.
The 5 major types of mucormycosis are:
- Rhino-orbital-cerebral disease – Patients present with unilateral facial pain, headaches, fever, nasal or sinus congestion and discharge, and black, necrotic ulcerations, usually involving the palate. Infection can erode locally and spread to the cavernous sinus, the internal carotid artery, and the brain. Orbital involvement can lead to orbital cellulitis, ophthalmoplegia, and multiple cranial nerve palsies, with a potential for permanent residual effects such as blindness and cranial nerve defects occurring up to 70% of the time. These patients may present with only a central retinal artery occlusion.
- Pulmonary disease – In the immunocompromised host, this can be insidiously and minimally symptomatic, often identified incidentally by chest CT or presenting with isolated fevers unresponsive to antibiotics. Some patients may develop cough, dyspnea, and unremitting fever despite broad-spectrum antibiotics. Hemoptysis occurs as a result of tissue necrosis and angio-invasion and, rarely, can be fatal. Physical examination findings are nonspecific and can include tachypnea, crackles, decreased breath sounds, and wheezing, although often the lung examination is normal.
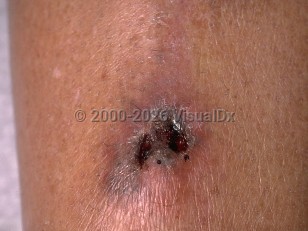
- Cutaneous disease – This form of mucormycosis may be primary or secondary. Primary infection may be associated with direct inoculation from trauma, burns, and surgical wounds. The affected tissue becomes inflamed, followed by subsequent necrosis. Secondary cutaneous mucormycosis occurs from hematogenous spread. Intertriginous cutaneous mucormycosis has been reported in immunocompromised patients who were hospitalized; lesions developed in skin folds seemingly in the absence of preexisting skin trauma.
- Gastrointestinal disease – This form is mainly seen in extreme cases of malnutrition or immunosuppression. It is believed to occur via direct ingestion of spores. Clinical findings may include abdominal pain, nausea, vomiting, gastrointestinal bleeding, fever, and change in bowel habits. It is the most common form of mucormycosis in newborns.
- Disseminated disease – This most commonly occurs following pulmonary mucormycosis, although it could be a result of any subtype. The brain is the most susceptible to infection, followed by the spleen, heart, skin, and other organs.
In patients with HIV, mucormycosis is rare, but when it does occur, it can do so without the typical predisposing factors. In patients with HIV / AIDS, mucormycosis tends to occur in those who use intravenous drugs, patients with prolonged and severe neutropenia, and individuals with very low CD4 counts. Systemic involvement can be severe and progress rapidly, or the disease can progress insidiously. Death frequently occurs. Mucormycosis may complicate previous bacterial infection.
In immunocompetent hosts, epidemic mucormycosis has been associated with penetrating and nonpenetrating trauma caused by natural disasters, for example, the tornado in Joplin, Missouri, in 2011. DNA analysis in that case showed an Apophysomyces trapeziformis species. In the wake of the COVID-19 pandemic, post-COVID-associated mucormycosis (predominantly pulmonary) has been reported with increasing frequency, particularly on the Indian subcontinent.
For discussion of diseases caused by fungi belonging to the order of Entomophthorales, see cutaneous basidiobolomycosis, disseminated basidiobolomycosis, and rhinofacial conidiobolomycosis.