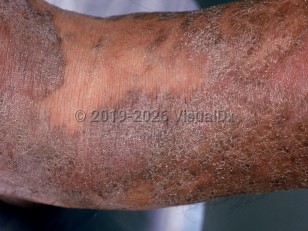
Non-AIDS-associated Kaposi sarcoma
Alerts and Notices
Important News & Links
Synopsis

Although KS is known to be an endothelial proliferation, it is unknown whether the growth is vascular or lymphatic in origin. It is also unknown whether KS is a hyperplastic lesion or a true neoplasm, as cell clonality studies are mixed. The exact mechanism of HHV-8's role in the disease is also not known, as not all individuals with HHV-8 infection develop KS.
Classic KS is seen almost exclusively in people of Mediterranean and Ashkenazi Jewish descent, with the age of onset typically between 50 and 70 years. The disease is slightly more common in men than women (ratio of 1-3:1). This type of KS most commonly runs an indolent course for several years, with slow enlargement of macules into plaques, nodules, or tumors and the gradual development of additional lesions. Lesions are most commonly on the legs. Some early lesions can regress, and others can progress, leading to clinical appearance of lesions in multiple stages. Up to one-third of the patients with classic KS develop a second primary malignancy, most frequently non-Hodgkin lymphoma.
African endemic KS largely affects males in equatorial Africa, with an incidence in endemic areas of 1%-10%. This represents significant disease burden in equatorial Africa, as 9% of all cancers in the area are endemic KS. There are 4 variants: nodular, florid, infiltrative, and lymphadenopathic. The florid and infiltrative types are aggressive. The lymphadenopathic type mostly affects children (with equal impact to boys and girls) and is fatal.
Iatrogenic KS results from long-term systemic immunosuppression from medications such as prednisone, cyclosporine, and calcineurin inhibitors. Incidence of KS in the post-transplant population is approximately < 1%-4%, and rates are lower in Western nations. This variant is mostly limited to the skin, with infrequent visceral involvement. Lesions may resolve when immunosuppressive medications are discontinued.
Lesions in all forms of KS may progress to involve or be present in other organs such as the lymph nodes, lungs, gastrointestinal (GI) tract, liver, and spleen. This is more likely to occur in advanced stages of the disease and more aggressive disease variants. Most visceral cases are asymptomatic, but GI bleeding can occur.
Related topic: skin cancer in organ transplant recipients
Codes
C46.0 – Kaposi's sarcoma of skin
SNOMEDCT:
703625002 – Kaposi sarcoma not associated with acquired immunodeficiency syndrome
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:11/20/2023