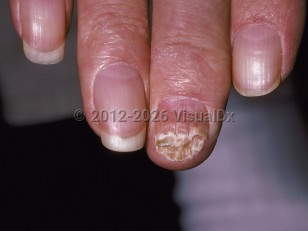
Onychomycosis - Nail and Distal Digit
Alerts and Notices
Important News & Links
Synopsis

Onychomycosis is a fungal infection of the nail (tinea unguium) caused by dermatophyte fungi and, less frequently, by nondermatophyte molds or yeasts. Onychomycosis is more frequent in men and is commonly associated with concurrent tinea pedis. The prevalence of onychomycosis in children varies from 0.2%-2.6% (mean 0.3%). The low prevalence in children compared with adults is thought to be due to children's fast nail plate growth and their lower incidence of tinea pedis compared with adults.
Predisposing factors include diabetes mellitus, peripheral vascular disease, immunosuppression, genetic predisposition, atopic dermatitis, psoriasis, Down syndrome, occlusive footwear, obesity, malignancy, trauma, and older age. Patients may also report a history of hyperhidrosis. A personal history of tinea pedis and/or contact with a household member with onychomycosis / tinea pedis are among the most common risk factors. Toenails are more commonly affected than fingernails, and fingernail infection is typically preceded by or associated with toenail infection. Onychomycosis is classified into 7 patterns based on the route of fungal invasion into the nail unit: distal lateral subungual, superficial, proximal subungual, endonyx, mixed pattern, totally dystrophic, and secondary onychomycosis.
Distal lateral subungual onychomycosis (DLSO) is the most common form of onychomycosis and begins with fungal invasion of the distal nail (hyponychium). In Western countries, DLSO is mainly due to Trichophyton rubrum.
Superficial onychomycosis (SO) is due to fungal invasion of the superficial dorsal nail plate, typically caused by T rubrum in HIV-infected patients and Trichophyton mentagrophytes in immunocompetent individuals. In children, superficial white onychomycosis (SWO) is typically caused by T rubrum. It accounts for 8%-28% of pediatric cases.
Proximal subungual onychomycosis (PSO) is caused by invasion of the proximal nail fold. In the absence of paronychia, PSO is typically due to T rubrum.
Endonyx onychomycosis (EO) presents as lamellar nail splitting and milky patches of the nail plate. The fungus directly invades the nail plate, but there is no penetration of the nail bed. The most common organisms are Trichophyton soudanense and Trichophyton violaceum.
Mixed pattern onychomycosis (MPO) occurs when there is more than one pattern of nail plate infection in the same nail. The most common patterns are PSO with SO or DLSO with SO.
Total dystrophic onychomycosis (TDO) presents as a crumbled nail plate and is the end stage of onychomycosis, typically DLSO.
Secondary onychomycosis occurs when fungi invade the nail plate secondary to other nonfungal nail diseases, such as psoriasis or prior trauma.
The dermatophytes T rubrum and T mentagrophytes are the first and second most common organisms in the United States. Other organisms include Microsporum canis and Trichophyton tonsurans.
Nondermatophyte molds are less commonly responsible for onychomycosis than dermatophytes. However, they are increasingly being recognized in warmer climates. Aspergillus, Acremonium, and Fusarium species and Scytalidium hyalinum may be responsible for DLSO, SO, and PSO; Scopulariopsis brevicaulis may present with brown-yellow nail plate discoloration; and Scytalidium dimidiatum typically presents with black nail discoloration.
When Candida species are cultured from nails, these species are not always the primary pathogen. Candida is commonly associated with chronic paronychia and occasionally secondarily infects the nail plate. True nail invasion by Candida is seen commonly in patients with chronic mucocutaneous candidiasis.
Immunocompromised Patient Considerations:
PSO has been reported to be more common in HIV infection and immunocompromised states.
Candida onychomycosis is seen in patients with chronic mucocutaneous candidiasis who are prone to direct invasion of Candida into their nail plate.
Infected nails may be the source of disseminated mycosis in immunosuppressed patients, especially those with hematologic malignancies or neutropenia.
Inherited deficiency (autosomal recessive) of CARD9 (caspase recruitment domain-containing protein 9), which is involved in the inflammatory cascade, may result in deep ulcerated fungal infections, Majocchi-like granulomas, severe tinea capitis and corporis, and onychomycosis. See CARD9 deficiency.
Predisposing factors include diabetes mellitus, peripheral vascular disease, immunosuppression, genetic predisposition, atopic dermatitis, psoriasis, Down syndrome, occlusive footwear, obesity, malignancy, trauma, and older age. Patients may also report a history of hyperhidrosis. A personal history of tinea pedis and/or contact with a household member with onychomycosis / tinea pedis are among the most common risk factors. Toenails are more commonly affected than fingernails, and fingernail infection is typically preceded by or associated with toenail infection. Onychomycosis is classified into 7 patterns based on the route of fungal invasion into the nail unit: distal lateral subungual, superficial, proximal subungual, endonyx, mixed pattern, totally dystrophic, and secondary onychomycosis.
Distal lateral subungual onychomycosis (DLSO) is the most common form of onychomycosis and begins with fungal invasion of the distal nail (hyponychium). In Western countries, DLSO is mainly due to Trichophyton rubrum.
Superficial onychomycosis (SO) is due to fungal invasion of the superficial dorsal nail plate, typically caused by T rubrum in HIV-infected patients and Trichophyton mentagrophytes in immunocompetent individuals. In children, superficial white onychomycosis (SWO) is typically caused by T rubrum. It accounts for 8%-28% of pediatric cases.
Proximal subungual onychomycosis (PSO) is caused by invasion of the proximal nail fold. In the absence of paronychia, PSO is typically due to T rubrum.
Endonyx onychomycosis (EO) presents as lamellar nail splitting and milky patches of the nail plate. The fungus directly invades the nail plate, but there is no penetration of the nail bed. The most common organisms are Trichophyton soudanense and Trichophyton violaceum.
Mixed pattern onychomycosis (MPO) occurs when there is more than one pattern of nail plate infection in the same nail. The most common patterns are PSO with SO or DLSO with SO.
Total dystrophic onychomycosis (TDO) presents as a crumbled nail plate and is the end stage of onychomycosis, typically DLSO.
Secondary onychomycosis occurs when fungi invade the nail plate secondary to other nonfungal nail diseases, such as psoriasis or prior trauma.
The dermatophytes T rubrum and T mentagrophytes are the first and second most common organisms in the United States. Other organisms include Microsporum canis and Trichophyton tonsurans.
Nondermatophyte molds are less commonly responsible for onychomycosis than dermatophytes. However, they are increasingly being recognized in warmer climates. Aspergillus, Acremonium, and Fusarium species and Scytalidium hyalinum may be responsible for DLSO, SO, and PSO; Scopulariopsis brevicaulis may present with brown-yellow nail plate discoloration; and Scytalidium dimidiatum typically presents with black nail discoloration.
When Candida species are cultured from nails, these species are not always the primary pathogen. Candida is commonly associated with chronic paronychia and occasionally secondarily infects the nail plate. True nail invasion by Candida is seen commonly in patients with chronic mucocutaneous candidiasis.
Immunocompromised Patient Considerations:
PSO has been reported to be more common in HIV infection and immunocompromised states.
Candida onychomycosis is seen in patients with chronic mucocutaneous candidiasis who are prone to direct invasion of Candida into their nail plate.
Infected nails may be the source of disseminated mycosis in immunosuppressed patients, especially those with hematologic malignancies or neutropenia.
Inherited deficiency (autosomal recessive) of CARD9 (caspase recruitment domain-containing protein 9), which is involved in the inflammatory cascade, may result in deep ulcerated fungal infections, Majocchi-like granulomas, severe tinea capitis and corporis, and onychomycosis. See CARD9 deficiency.
Codes
ICD10CM:
B35.1 – Tinea unguium
SNOMEDCT:
414941008 – Onychomycosis
B35.1 – Tinea unguium
SNOMEDCT:
414941008 – Onychomycosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/25/2020
Last Updated:01/15/2025
Last Updated:01/15/2025
 Patient Information for Onychomycosis - Nail and Distal Digit
Patient Information for Onychomycosis - Nail and Distal Digit
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Onychomycosis - Nail and Distal Digit