Emergency: requires immediate attention
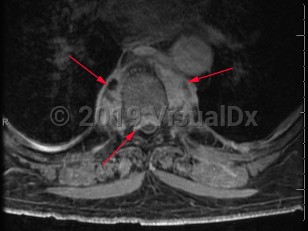
Paraspinal abscess
Alerts and Notices
Important News & Links
Synopsis

Paraspinal abscess is a collection of pus located around the spinal cord. This is usually seen as a complication of vertebral osteomyelitis and discitis (diskitis) but may be related to hematogenous seeding during bloodstream infection. Epidural catheters and injections may lead to direct inoculation of the epidural space. Frequently, the location of the abscess is in the epidural space.
The most common offending pathogens are gram-positive organisms, including Staphylococcus aureus. Gram-negative infections can occur and are often associated with ascending urinary sources. If epidemiologic risk factors are present, the clinician should also consider infection due to tuberculosis. Less common pathogens include Nocardia, Actinomyces species, and fungi.
Patients may have acute (develops over hours) or subacute (develops over weeks to months) back pain. Fever may or may not be present. As the abscess forms, patients typically have focal and severe back pain. As the size of the abscess increases, it may impinge on the spinal cord, leading to signs of spinal cord compression, including motor weakness and sensory deficits. Untreated, the patient's neurologic symptoms can worsen to the point of irreversible paralysis.
Diagnosis is typically made after the patient undergoes surgical drainage of the abscess. Infective material can be cultured to establish a diagnosis. Common laboratory findings include leukocytosis and elevation in inflammatory markers (sedimentation rate or C-reactive protein). Concomitant bloodstream infection may be present.
Risk factors include preceding back surgery, spinal surgery or instrumentation, back injury, and bacteremia. Patients at increased risk include injection drug users, immunosuppressed patients, and individuals with diabetes.
The most common offending pathogens are gram-positive organisms, including Staphylococcus aureus. Gram-negative infections can occur and are often associated with ascending urinary sources. If epidemiologic risk factors are present, the clinician should also consider infection due to tuberculosis. Less common pathogens include Nocardia, Actinomyces species, and fungi.
Patients may have acute (develops over hours) or subacute (develops over weeks to months) back pain. Fever may or may not be present. As the abscess forms, patients typically have focal and severe back pain. As the size of the abscess increases, it may impinge on the spinal cord, leading to signs of spinal cord compression, including motor weakness and sensory deficits. Untreated, the patient's neurologic symptoms can worsen to the point of irreversible paralysis.
Diagnosis is typically made after the patient undergoes surgical drainage of the abscess. Infective material can be cultured to establish a diagnosis. Common laboratory findings include leukocytosis and elevation in inflammatory markers (sedimentation rate or C-reactive protein). Concomitant bloodstream infection may be present.
Risk factors include preceding back surgery, spinal surgery or instrumentation, back injury, and bacteremia. Patients at increased risk include injection drug users, immunosuppressed patients, and individuals with diabetes.
Codes
ICD10CM:
G06.1 – Intraspinal abscess and granuloma
SNOMEDCT:
11980001000004100 – Paraspinal abscess
G06.1 – Intraspinal abscess and granuloma
SNOMEDCT:
11980001000004100 – Paraspinal abscess
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/30/2016
Last Updated:08/06/2023
Last Updated:08/06/2023
Emergency: requires immediate attention
Paraspinal abscess