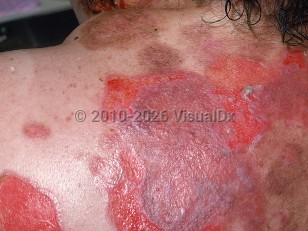
Pemphigus vulgaris - Oral Mucosal Lesion
See also in: Overview,AnogenitalAlerts and Notices
Important News & Links
Synopsis

The estimated incidence worldwide is 0.76-5 cases per million per year, although PV occurs in higher incidences in individuals of Jewish ancestry, as well as in certain geographic areas (Middle East, Southeastern Europe, and India). Variants of the ST18 gene have been found to confer increased risk of PV in some populations. PV is typically a disease of adults, with average age of onset between 40 and 60 years, but PV rarely can occur in childhood and young adulthood. There does not appear to be a consistent sex predilection.
Almost all patients with PV develop painful erosions on the oral mucosa, and individuals with the mucocutaneous type develop flaccid bullae and erosions on the skin. Before the introduction of systemic corticosteroids, the mortality of PV was 75%. Still, severe cases of PV can be life-threatening, and complications can be related immunosuppression from drugs used to treat severe PV, secondary infections, loss of the skin barrier, and poor oral intake.
Patients usually complain of painful sores in the mouth and bleeding gums when brushing their teeth. Lesions most likely involve the palatine and buccal mucosa. Lesions can rarely extend to the vermillion of the lips. Involvement of the throat may cause sore throat, pain with swallowing, and hoarseness. In severe disease, involvement of the entire esophagus has been reported. The oral cavity is frequently the first site of involvement, with painful skin lesions sometimes appearing months or years later. Other mucosal sites that may be involved include the nasal mucosa, throat, eyes, and genital areas.
Codes
L10.0 – Pemphigus vulgaris
SNOMEDCT:
49420001 – Pemphigus vulgaris
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:01/10/2022
 Patient Information for Pemphigus vulgaris - Oral Mucosal Lesion
Patient Information for Pemphigus vulgaris - Oral Mucosal Lesion- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient