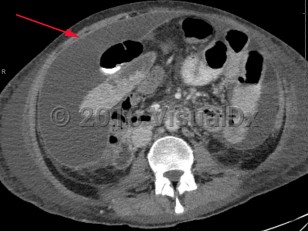
- Primary (spontaneous) bacterial peritonitis – Occurs without an apparent source of contamination and is thought to be secondary to bacterial translocation across the bowel. It is most commonly found in patients with underlying cirrhosis and ascites, but may be found in patients with congestive heart failure, systemic lupus erythematosus, chronic viral hepatitis, or acute viral hepatitis. Presentation can be subtle, and up to 30% of patients may be asymptomatic. Fever is common, but presentation can be marked by altered mental status or abdominal pain in those with cirrhosis. This infection is often paucibacillary, and culture is not uncommonly negative. When an organism is identified, common organisms include Escherichia coli, streptococci, enterococci, and pneumococci.
- Secondary peritonitis – Results from the contamination of the peritoneum from spillage from an intraabdominal viscus, and results in gradually worsening abdominal pain as the parietal peritoneum becomes irritated. Pain, fever, and guarding are common presenting symptoms. Polymicrobial infections are common, including gram positive, gram negative, and anaerobes.
- Peritonitis secondary to ambulatory peritoneal dialysis (PD) – Presents with fever, diffuse abdominal pain, purulence at PD catheter site, guarding, and cloudy peritoneal fluid. Pathogens responsible are commonly skin flora such as Staphylococcus organisms.
Peritonitis
Alerts and Notices
Important News & Links
Synopsis

Inflammation of the visceral and parietal peritoneum resulting in acute, severe abdominal pain with fever and diffuse abdominal tenderness with rigidity and guarding, most often secondary to an infectious or inflammatory process. Peritonitis can be primary, secondary, or a result of continuous peritoneal dialysis:
Codes
ICD10CM:
K65.9 – Peritonitis, unspecified
SNOMEDCT:
48661000 – Peritonitis
K65.9 – Peritonitis, unspecified
SNOMEDCT:
48661000 – Peritonitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/19/2017
Last Updated:01/18/2021
Last Updated:01/18/2021