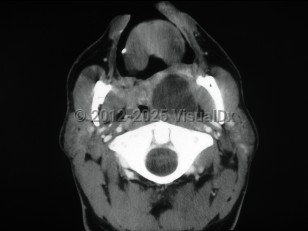
Peritonsillar abscess
Alerts and Notices
Important News & Links
Synopsis

Peritonsillar abscess, also known as quinsy, is a deep neck space infection characterized by a collection of pus in the peritonsillar space.
This infection develops as a suppurative complication of acute tonsillitis or pharyngitis.
As with other deep neck space infections, peritonsillar abscesses are frequently polymicrobial in nature and consist of mouth flora. Some important pathogens to consider when choosing empiric antibiotics include Group A Streptococcus, Staphylococcus aureus, Haemophilus, and Fusobacterium.
Patients present with a muffled voice, fever, sore throat, and dysphagia. There is deviation of the uvula to the unaffected side. Trismus and otalgia may be present. This infection usually affects young adults, but all ages can be affected. Older adults may have subtler symptoms. Laboratory findings include leukocytosis. Treatment consists of antibiotic therapy and surgical drainage.
Complications of this infection include airway obstruction or extension of the infection into contiguous spaces in the neck.
This infection develops as a suppurative complication of acute tonsillitis or pharyngitis.
As with other deep neck space infections, peritonsillar abscesses are frequently polymicrobial in nature and consist of mouth flora. Some important pathogens to consider when choosing empiric antibiotics include Group A Streptococcus, Staphylococcus aureus, Haemophilus, and Fusobacterium.
Patients present with a muffled voice, fever, sore throat, and dysphagia. There is deviation of the uvula to the unaffected side. Trismus and otalgia may be present. This infection usually affects young adults, but all ages can be affected. Older adults may have subtler symptoms. Laboratory findings include leukocytosis. Treatment consists of antibiotic therapy and surgical drainage.
Complications of this infection include airway obstruction or extension of the infection into contiguous spaces in the neck.
Codes
ICD10CM:
J36 – Peritonsillar abscess
SNOMEDCT:
15033003 – Peritonsillar abscess
J36 – Peritonsillar abscess
SNOMEDCT:
15033003 – Peritonsillar abscess
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:01/18/2021