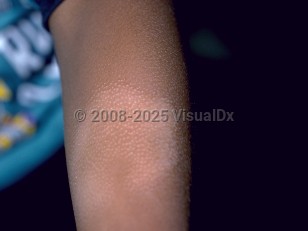
Pityriasis alba in Infant/Neonate
Alerts and Notices
Important News & Links
Synopsis

Pityriasis alba is a common condition primarily affecting children, but not exclusively, and especially those with atopic diathesis (eg, asthma, allergic rhinitis and conjunctivitis, atopic dermatitis). Classic pityriasis alba is characterized by ill-defined hypopigmented macules or patches, ranging in size from 0.5-5 cm, occurring on the face or upper body. Lesions may be asymptomatic or mildly pruritic.
Pityriasis alba often has a chronic course, tends to relapse, and usually worsens in the summer with increased sun exposure. It predominately occurs in children between the ages of 3 and 16 years and is found equally in both sexes. In the majority of patients, spontaneous resolution typically occurs before adulthood. This disorder is common in all ethnicities, although the hypopigmented lesions are more obvious in patients with darker skin colors.
The exact cause of the condition is unknown, although the characteristic hypopigmentation may be secondary to a preceding subclinical dermatitis. Environmental triggers such as heat, humidity, sunlight exposure, detergents / soaps, abrasive clothing, chemicals, and smoke, along with stress, may aggravate this disorder. Microorganisms such as Pityrosporum, Streptococcus, Aspergillus, and Staphylococcus may also be triggers. Evidence also suggests that pityriasis alba is a mild eczematous dermatitis.
Pityriasis alba often has a chronic course, tends to relapse, and usually worsens in the summer with increased sun exposure. It predominately occurs in children between the ages of 3 and 16 years and is found equally in both sexes. In the majority of patients, spontaneous resolution typically occurs before adulthood. This disorder is common in all ethnicities, although the hypopigmented lesions are more obvious in patients with darker skin colors.
The exact cause of the condition is unknown, although the characteristic hypopigmentation may be secondary to a preceding subclinical dermatitis. Environmental triggers such as heat, humidity, sunlight exposure, detergents / soaps, abrasive clothing, chemicals, and smoke, along with stress, may aggravate this disorder. Microorganisms such as Pityrosporum, Streptococcus, Aspergillus, and Staphylococcus may also be triggers. Evidence also suggests that pityriasis alba is a mild eczematous dermatitis.
Codes
ICD10CM:
L30.5 – Pityriasis alba
SNOMEDCT:
402296004 – Pityriasis alba
L30.5 – Pityriasis alba
SNOMEDCT:
402296004 – Pityriasis alba
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:06/11/2024
Last Updated:06/30/2024
Last Updated:06/30/2024
 Patient Information for Pityriasis alba in Infant/Neonate
Patient Information for Pityriasis alba in Infant/Neonate
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Pityriasis alba in Infant/Neonate