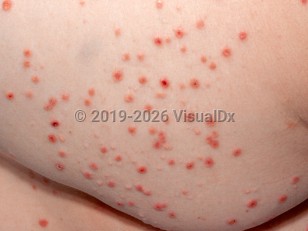
Pityriasis lichenoides et varioliformis acuta in Infant/Neonate
Alerts and Notices
Important News & Links
Synopsis

A variant of PLEVA, febrile ulceronecrotic Mucha-Habermann disease (FUMHD), is marked by larger, more ulcerative, and necrotic lesions along with fever and arthralgia. There may be gastrointestinal, pulmonary, and central nervous system (CNS) involvement.
Pityriasis lichenoides chronica (PLC) is a related but more chronic form that is considered to be on a continuum with PLEVA. In contrast to the crusts, vesicles, and pustules seen in PLEVA, PLC takes on a more indolent course and is characterized by crops of scaly, erythematous papules that spontaneously regress over months to years. Overlapping cases of PLEVA and PLC do occur.
PLEVA is generally viewed as a benign lymphoproliferative disorder that lasts approximately 1-3 years. Duration has been associated with the distribution of lesions. Cases with diffuse skin involvement tend to have a shorter, approximately 11-month course, while acral-dominant cases have a longer course of approximately 33 months. Cases with a central distribution fall between these extremes.
The etiology of PLEVA is unknown but may be a lymphoproliferative response to a foreign antigen as it has been associated with viral infections, drugs, vaccinations, and radiocontrast dyes. There are case reports of progression to cutaneous T-cell lymphoma (CTCL). No guidelines have been established for monitoring this possible progression.
Codes
L41.0 – Pityriasis lichenoides et varioliformis acuta
SNOMEDCT:
86487001 – Acute lichenoid pityriasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:09/03/2019