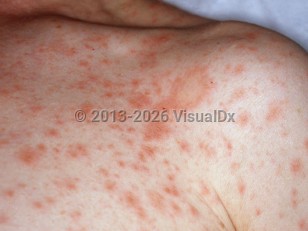
Pityriasis rosea in Infant/Neonate
Alerts and Notices
Important News & Links
Synopsis

Pityriasis rosea is usually pruritic in pediatric patients, although it may also be asymptomatic. Constitutional symptoms may precede the eruption, including irritability, fever, headache, sore throat, and cough. In most pediatric patients, the rash typically resolves within 2-6 weeks. Recurrence is rare.
Adolescents and young adults are most commonly affected. Pityriasis rosea is less common in children younger than 10 years, and it is rare in children younger than 2 years. An atypical form of pityriasis rosea, characterized by papular lesions and facial and scalp involvement, is more prevalent in Black children. In individuals with darker skin colors, hyperpigmentation can result upon resolution.
While the exact cause remains unclear, pityriasis rosea in children is thought to be associated with primary infection or systemic reactivation of human herpesvirus 6 and 7 (HHV-6 and HHV-7).
Certain drugs can cause a pityriasiform eruption that resembles pityriasis rosea. Drug-related pityriasis rosea-like lesions may appear more red-violet in color, typically do not present with a herald patch, and may be associated with eosinophilia. Pityriasis rosea may also occur after vaccines, such as the COVID-19, smallpox, tuberculosis, and human papillomavirus (HPV) vaccines.
Codes
L42 – Pityriasis rosea
SNOMEDCT:
77252004 – Pityriasis rosea
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:12/05/2023
 Patient Information for Pityriasis rosea in Infant/Neonate
Patient Information for Pityriasis rosea in Infant/Neonate- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient