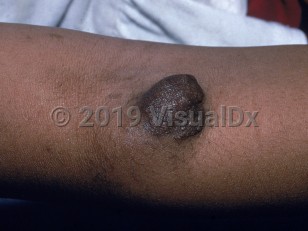
Plexiform neurofibroma in Infant/Neonate
Alerts and Notices
Important News & Links
Synopsis

Plexiform neurofibromas (PNF) are benign tumors arising from cells of the nerve sheath. Such tumors grow along the length of the nerve, often involving multiple branches. PNF are likely congenital in origin but do not become clinically apparent for several years, typically between ages 3-5 years, although onset after birth and in adulthood have been described. Solitary lesions may be the result of NF1 gene mosaicism or loss of heterozygosity.
PNF are associated with neurofibromatosis type I (NF1) and are considered pathognomonic for this condition. A single plexiform neurofibroma is a single criterion for NF1 (at least 2 of 7 criteria are required for diagnosis). About one-fourth of children with NF1 develop PNF. Facial PNF usually appear within the first 3 years of life and often involve the trigeminal nerve.
Unlike cutaneous and subcutaneous neurofibromas, PNF are unaffected by hormonal changes during puberty or pregnancy. PNF may be asymptomatic but may also cause morbidity because of a propensity to infiltrate surrounding tissue. Complications arise from compression of surrounding structures, which can induce pain, neurologic impairment, and motor dysfunction and cause disfigurement. Rarely, PNF can result in death from such complications. PNF carry an approximate 10% risk of developing into malignant peripheral nerve sheath tumors.
PNF are associated with neurofibromatosis type I (NF1) and are considered pathognomonic for this condition. A single plexiform neurofibroma is a single criterion for NF1 (at least 2 of 7 criteria are required for diagnosis). About one-fourth of children with NF1 develop PNF. Facial PNF usually appear within the first 3 years of life and often involve the trigeminal nerve.
Unlike cutaneous and subcutaneous neurofibromas, PNF are unaffected by hormonal changes during puberty or pregnancy. PNF may be asymptomatic but may also cause morbidity because of a propensity to infiltrate surrounding tissue. Complications arise from compression of surrounding structures, which can induce pain, neurologic impairment, and motor dysfunction and cause disfigurement. Rarely, PNF can result in death from such complications. PNF carry an approximate 10% risk of developing into malignant peripheral nerve sheath tumors.
Codes
ICD10CM:
D36.10 – Benign neoplasm of peripheral nerves and autonomic nervous system, unspecified
SNOMEDCT:
403818001 – Plexiform neurofibroma
D36.10 – Benign neoplasm of peripheral nerves and autonomic nervous system, unspecified
SNOMEDCT:
403818001 – Plexiform neurofibroma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:11/27/2023