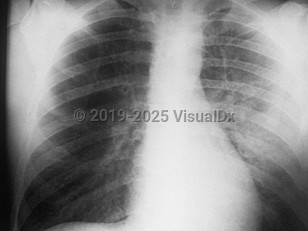
Rapid patient isolation, use of personal protective equipment for health care workers, antibiotic delivery, and notification of public health professionals are essential preliminary steps when the disease is suspected. Supportive care in the intensive care unit may be necessary. Patients may require respiratory support and mechanical ventilation as well as fluid resuscitation and blood pressure support.
- Antibiotic treatment should begin as soon as plague is suspected. Pretreatment samples (blood, sputum, lymph node / bubo aspirates) should be collected if possible but should NOT delay treatment.
- Control measures and personal protective equipment for health care workers should be geared toward droplet transmission at a minimum. Consult infection control experts to determine whether additional protection is warranted for caring for patients with potential aerosolizing interventions (eg, high-flow nasal cannula supplemental oxygen delivery).
Infection with the gram-negative bacillus Yersinia pestis can lead to a highly lethal disease, commonly referred to as the plague, that requires early recognition and prompt treatment. The pneumonic form of plague is characterized by a severe and rapidly progressive pneumonia. Yersinia pestis infection can also manifest as bubonic and septicemic forms. Bubonic plague is the most common form of the disease in humans.
The reservoir for Y pestis is most commonly rodents (eg, prairie dogs, squirrels, chipmunks, rats), although cases involving dogs and cats have been described as well. The vectors are fleas that feed on the infected animals and then can transmit the bacteria to susceptible hosts such as humans.
Pneumonic plague has both a primary and a secondary form. The primary form is contracted from inhaling aerosolized droplets from an infected person and occurs in only about 3% of plague-infected patients. These droplets do not remain suspended in the air for a prolonged period of time after exhalation and require close contact (less than or equal to 6 feet [1.8 meters]) for transmission. Secondary pneumonic plague occurs when infection beginning outside of the lungs, such as from bubonic or septicemic plague, disseminates to the lungs; approximately 12% of such cases progress to pneumonic form. Bubonic and septicemic plague are rarely transmissible from human to human but may become transmissible via droplets once in the pneumonic stage.
The incubation period can range from 1-6 days (average 2-4 days) and may be shorter (1-3 days) for the primary pneumonic form.
Primary pneumonic plague results in a severe fulminant illness with high fever, chills, headache, productive cough, chest pain, hemoptysis, extreme malaise, myalgias, tachypnea, tachycardia, and pneumonia. Gastrointestinal symptoms, including nausea, vomiting, abdominal pain, and diarrhea are also commonly seen. Secondary pneumonic plague is equally severe but arises later in the disease course of a patient initially presenting with bubonic or septicemic plague.
If not treated within 24 hours of onset, pneumonic plague rapidly progresses to acral cyanosis, respiratory failure, septicemia, circulatory collapse, and death. Untreated, the mortality rate of pneumonic plague approaches 100%. With treatment, the rate drops to 17%-20%.
It is important to recognize that initial symptoms of primary pneumonic plague may be similar to more common causes of pneumonia and that the initial symptoms of bubonic and septicemic plague can also be initially nonspecific. The clinician must have a high index of suspicion based on endemic locations, recent travel, and close contact with ill individuals or with rodents or domestic animals that have recently become sick.
Initial diagnosis in the emergency department for a single case may be difficult. Unless the link to exposure is readily apparent, most cases will be diagnosed after admission based on microbiologic culture data or PCR (sputum or blood). Human-to-human transmission is possible, so if pneumonic plague is suspected, infection control practices must be rapidly implemented. Control measures and personal protective equipment for health care workers should be geared toward droplet transmission at a minimum. Consult infection control experts to determine whether additional protection is warranted for caring for patients with potential aerosolizing interventions (eg, high-flow nasal cannula supplemental oxygen delivery).
Endemic plague is seen in the western United States (Colorado, New Mexico, Arizona, California, southern Oregon, and Nevada) as well as in central and southern Africa (Democratic Republic of Congo, Uganda, Madagascar), parts of South America (Peru), and central Asia and the Indian subcontinent. The incidence is likely higher than reported given that the majority of cases happen in underdeveloped regions of the world where reporting mechanisms are lacking. Naturally occurring pneumonic plague is uncommon. Hikers, campers, veterinarians, and owners of infected animals, especially those living or visiting endemic areas, are at higher risk for contracting plague.
Pneumonic plague is classified as a Category A bioterrorism agent because of its ease of dissemination, contagiousness, and high mortality rate. The most likely method of dispersal would be as an aerosol, but simply having an infected individual walk around infecting others is another possible mode of dissemination, albeit less efficient at making many persons ill. Concern for bioterrorism should be raised if multiple patients arrive with similar symptoms suspicious for plague.
Rapid patient isolation, use of personal protective equipment for health care workers, antibiotic delivery, and notification of public health professionals are essential preliminary steps when the disease is suspected. If bioterrorism is suspected, the clinician should have a low threshold to activate the hospital incident command system and notify public health authorities.
If the outbreak is intentional and pneumonic plague is occurring in the community, all patients with rapidly progressive pneumonia should be considered to have pneumonic plague unless an alternate diagnosis is found.