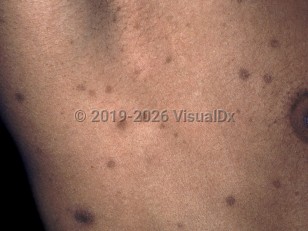
Postinflammatory hyperpigmentation in Child
Alerts and Notices
Important News & Links
Synopsis

Postinflammatory hyperpigmentation (PIH) describes localized darker skin areas as a consequence of trauma and/or inflammation. It can arise in all skin types but affects patients with darker skin phototypes with greater frequency and severity. There is no age or sex predilection.
The inflammatory process may be incited by an infection, allergy, drug reaction, mechanical or thermal injury, phototoxic eruption, or an intrinsic skin disease.
Although clinically benign, patches of PIH can cause significant cosmetic and psychosocial distress.
Inflammation may induce overproduction of melanin in the epidermis through the effect of inflammatory mediators such as metabolites of arachidonic acid and reactive oxygen species. PIH in the dermis results from damage to basal keratinocytes with release of melanin subsequently phagocytosed by dermal macrophages. Most lesions are a combination of epidermal and dermal pigmentation, the latter being more difficult to treat.
The lesions of PIH may be accentuated by sunlight.
The inflammatory process may be incited by an infection, allergy, drug reaction, mechanical or thermal injury, phototoxic eruption, or an intrinsic skin disease.
Although clinically benign, patches of PIH can cause significant cosmetic and psychosocial distress.
Inflammation may induce overproduction of melanin in the epidermis through the effect of inflammatory mediators such as metabolites of arachidonic acid and reactive oxygen species. PIH in the dermis results from damage to basal keratinocytes with release of melanin subsequently phagocytosed by dermal macrophages. Most lesions are a combination of epidermal and dermal pigmentation, the latter being more difficult to treat.
The lesions of PIH may be accentuated by sunlight.
Codes
ICD10CM:
L81.0 – Postinflammatory hyperpigmentation
SNOMEDCT:
238699007 – Post-inflammatory hyperpigmentation
L81.0 – Postinflammatory hyperpigmentation
SNOMEDCT:
238699007 – Post-inflammatory hyperpigmentation
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/12/2019
Last Updated:09/12/2019
Last Updated:09/12/2019
 Patient Information for Postinflammatory hyperpigmentation in Child
Patient Information for Postinflammatory hyperpigmentation in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Postinflammatory hyperpigmentation in Child