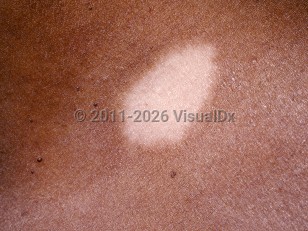
Postinflammatory hypopigmentation in Adult
Alerts and Notices
Important News & Links
Synopsis

Postinflammatory hypopigmentation is the presence of partial or total loss of pigmentation that occurs after resolution of cutaneous inflammation or after trauma.
Postinflammatory hypopigmentation can occur in patients of all ages, sexes, and skin types, and is more visibly pronounced in those with darker skin phototypes. It can be seen as a sequela of many inflammatory skin diseases (atopic dermatitis, seborrheic dermatitis, psoriasis, lichen striatus, pityriasis lichenoides chronica, lichen planus, sarcoidosis, discoid lupus erythematosus), infections (zoster, pityriasis versicolor, impetigo), procedures (chemical peels, laser, dermabrasion), and burns.
Time to resolution of hypopigmentation is dependent on the underlying cause and severity of inflammation, ranging from a few weeks in minimally hypopigmented lesions to several years in depigmented lesions (eg, discoid lupus erythematosus and burns).
Related topic: Drug-induced hypopigmentation
Postinflammatory hypopigmentation can occur in patients of all ages, sexes, and skin types, and is more visibly pronounced in those with darker skin phototypes. It can be seen as a sequela of many inflammatory skin diseases (atopic dermatitis, seborrheic dermatitis, psoriasis, lichen striatus, pityriasis lichenoides chronica, lichen planus, sarcoidosis, discoid lupus erythematosus), infections (zoster, pityriasis versicolor, impetigo), procedures (chemical peels, laser, dermabrasion), and burns.
Time to resolution of hypopigmentation is dependent on the underlying cause and severity of inflammation, ranging from a few weeks in minimally hypopigmented lesions to several years in depigmented lesions (eg, discoid lupus erythematosus and burns).
Related topic: Drug-induced hypopigmentation
Codes
ICD10CM:
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
277787003 – Post-inflammatory hypopigmentation
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
277787003 – Post-inflammatory hypopigmentation
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:12/12/2019
Last Updated:12/12/2019
Last Updated:12/12/2019
 Patient Information for Postinflammatory hypopigmentation in Adult
Patient Information for Postinflammatory hypopigmentation in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Postinflammatory hypopigmentation in Adult