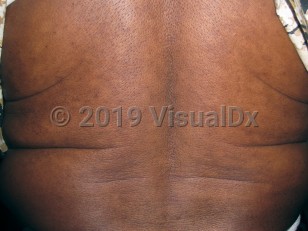
Progressive macular hypomelanosis
Alerts and Notices
Important News & Links
Synopsis

Progressive macular hypomelanosis (PMH) is a common pigmentary disorder resulting in hypopigmentation of the skin. It has also been called cutis trunci variata, nummular and confluent hypomelanosis, Creole dyschromia, and idiopathic multiple large-macule hypomelanosis.
PMH is characterized by numerous hypopigmented macules and patches that affect primarily the lumbar region and abdomen. Rarely, the condition extends to proximal limbs and the neck. While classically absent from the face, rare facial lesions have been described. The hypopigmented macules are ill-defined, nummular, symmetric, and without scale. The lesions are asymptomatic without history of preceding infection, inflammation, or injury.
PMH may last for years, but typically it resolves before age 40. The condition chiefly affects adolescents and young adults, particularly women aged 13-38 years. PMH affects all populations worldwide, but it is more common in tropical regions and in patients with darker skin colors.
The pathogenesis of PMH is unknown. However, studies have suggested that the hypopigmentation may be due to Cutibacterium acnes (formerly known as Propionibacterium acnes). This bacterium is found in the sebum of the pilosebaceous duct within hypopigmented lesions. The precise mechanism by which C acnes causes hypopigmentation is unclear, but it is hypothesized that the organism produces a substance that interferes with melanogenesis and/or melanosome distribution. More recent studies suggest that C acnes subspecies elongatum (type III) may more specifically be associated with PMH, as PMH rarely affects the face and C acnes type III rarely colonizes the face.
PMH is characterized by numerous hypopigmented macules and patches that affect primarily the lumbar region and abdomen. Rarely, the condition extends to proximal limbs and the neck. While classically absent from the face, rare facial lesions have been described. The hypopigmented macules are ill-defined, nummular, symmetric, and without scale. The lesions are asymptomatic without history of preceding infection, inflammation, or injury.
PMH may last for years, but typically it resolves before age 40. The condition chiefly affects adolescents and young adults, particularly women aged 13-38 years. PMH affects all populations worldwide, but it is more common in tropical regions and in patients with darker skin colors.
The pathogenesis of PMH is unknown. However, studies have suggested that the hypopigmentation may be due to Cutibacterium acnes (formerly known as Propionibacterium acnes). This bacterium is found in the sebum of the pilosebaceous duct within hypopigmented lesions. The precise mechanism by which C acnes causes hypopigmentation is unclear, but it is hypothesized that the organism produces a substance that interferes with melanogenesis and/or melanosome distribution. More recent studies suggest that C acnes subspecies elongatum (type III) may more specifically be associated with PMH, as PMH rarely affects the face and C acnes type III rarely colonizes the face.
Codes
ICD10CM:
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
37257004 – Decreased melanin pigmentation
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
37257004 – Decreased melanin pigmentation
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:04/18/2023
Last Updated:04/19/2023
Last Updated:04/19/2023