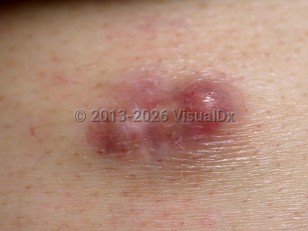
Proliferating pilar tumor
Alerts and Notices
Important News & Links
Synopsis

Proliferating trichilemmal tumor (PTT), also known as proliferating pilar tumor / cyst, is an uncommon benign dermal neoplasm that arises from the outer root sheath of the hair follicle. It is presumed to develop from a pre-existing trichilemmal (pilar) cyst.
PTT is more common among individuals of Northern European descent and is seen most often (approximately 90% of cases) on the scalp, typically in women in their fifth or sixth decade. Isolated cases inherited in an autosomal dominant fashion have been reported.
The malignant transformation of PTT is very rare. Only a small number of malignant proliferating trichilemmal tumor (MPTT) cases with documented invasion and metastasis have been reported. Malignant transformation may be preceded by rapid growth, necrosis, and ulceration.
PTT is more common among individuals of Northern European descent and is seen most often (approximately 90% of cases) on the scalp, typically in women in their fifth or sixth decade. Isolated cases inherited in an autosomal dominant fashion have been reported.
The malignant transformation of PTT is very rare. Only a small number of malignant proliferating trichilemmal tumor (MPTT) cases with documented invasion and metastasis have been reported. Malignant transformation may be preceded by rapid growth, necrosis, and ulceration.
Codes
ICD10CM:
L72.12 – Trichilemmal cyst
SNOMEDCT:
254678009 – Proliferating pilar cyst
L72.12 – Trichilemmal cyst
SNOMEDCT:
254678009 – Proliferating pilar cyst
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:06/12/2019
Last Updated:06/19/2019
Last Updated:06/19/2019
Proliferating pilar tumor