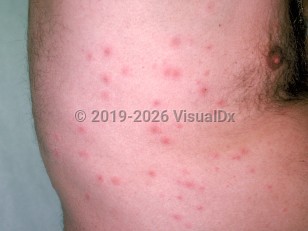
Pseudomonas folliculitis in Adult
Alerts and Notices
Important News & Links
Synopsis

Pseudomonas folliculitis, or hot tub folliculitis, is an infection of hair follicles with Pseudomonas bacteria. Outbreaks occur in people after exposure to a contaminated spa, swimming pool, hot tub, or water in the workplace. It is also associated with the use of contaminated water-associated objects, such as loofah sponges, swimming pool inflatables, rubber gloves, and nylon towels. Many outbreaks have been associated with inadequate chlorine levels. However, Pseudomonas is able to grow within biofilms despite normal chlorination. It also can be seen with higher incidence in patients on long-term antibiotic therapy for acne vulgaris.
Clinically, Pseudomonas folliculitis is characterized by tender or pruritic folliculocentric papules preferentially localized to the trunk, buttocks, and extremities. Inflammation of Montgomery's follicles of the breast has also been described in one outbreak in Alaska. Symptoms typically develop within 1-4 days after exposure to the contaminated water source. Infection can be associated with mild fever, malaise, lymphadenopathy, and leukocytosis. The cutaneous eruption usually fades within 7-14 days without therapy.
Water sources contaminated with Pseudomonas are also associated with outbreaks of painful plantar nodules termed the Pseudomonas hot-foot syndrome. These patients may or may not have a concomitant folliculitis.
There is no geographic distribution of Pseudomonas folliculitis. However, since hot tubs and natural hot springs are common activities of travelers and since pyodermas (purulent skin diseases) are among the most frequently reported complaints in returning travelers, a high degree of clinical suspicion is warranted.
Clinically, Pseudomonas folliculitis is characterized by tender or pruritic folliculocentric papules preferentially localized to the trunk, buttocks, and extremities. Inflammation of Montgomery's follicles of the breast has also been described in one outbreak in Alaska. Symptoms typically develop within 1-4 days after exposure to the contaminated water source. Infection can be associated with mild fever, malaise, lymphadenopathy, and leukocytosis. The cutaneous eruption usually fades within 7-14 days without therapy.
Water sources contaminated with Pseudomonas are also associated with outbreaks of painful plantar nodules termed the Pseudomonas hot-foot syndrome. These patients may or may not have a concomitant folliculitis.
There is no geographic distribution of Pseudomonas folliculitis. However, since hot tubs and natural hot springs are common activities of travelers and since pyodermas (purulent skin diseases) are among the most frequently reported complaints in returning travelers, a high degree of clinical suspicion is warranted.
Codes
ICD10CM:
L73.8 – Other specified follicular disorders
SNOMEDCT:
402921005 – Pseudomonas aeruginosa folliculitis
L73.8 – Other specified follicular disorders
SNOMEDCT:
402921005 – Pseudomonas aeruginosa folliculitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/21/2018
Last Updated:10/21/2018
Last Updated:10/21/2018
 Patient Information for Pseudomonas folliculitis in Adult
Patient Information for Pseudomonas folliculitis in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Pseudomonas folliculitis in Adult