The etiology of the disease is multifactorial, with both genetic and environmental factors. PsA affects men and women equally and is predominantly seen in white individuals, similar to psoriasis.
Symptoms:
- Pain, stiffness in affected joints, with joint stiffness present for > 30 minutes in the morning (after waking) or after prolonged inactivity. Improves with activity (versus osteoarthritis / degenerative joint disease, which typically worsens with activity).
- With axial involvement – Inflammatory back pain and stiffness that improve with activity; night symptoms can cause waking from sleep; decreased range of motion of the axial spine and neck over time.
- Tender / painful; swelling at entheses (sites of tendon insertion into bone).
- Tendonitis / tenosynovitis
- Ocular inflammation may lead to scleral erythema, dry eye / foreign body sensation, or uveitis with potential visual disturbance and pain.
- Hearing loss is increased in patients with PsA.
- Tender, painful, swollen joints with possible erythema, effusion, and warmth noted in more actively inflamed joints.
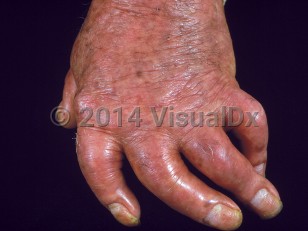
- Dactylitis – Inflammation and swelling of the entire digit including metacarpophalangeal (MCP) through proximal / distal interphalangeal (PIP/DIP) joints and intervening soft tissue, giving a "sausage digit" appearance.
- Enthesitis – Inflammation at tendinous insertion into bone, with tenderness.
- Distal (DIP) arthritis
- Oligoarthritis, asymmetric
- Rheumatoid arthritis (RA)-like symmetrical polyarthritis
- Arthritis mutilans – aggressive, destructive phenotype
- Axial spondylitis, sacroiliitis
Risk factors:
- Patients with nail, scalp, and inverse (intertriginous) psoriatic skin disease have a higher risk of developing PsA.
- Several genetic risk markers (HLA associations) are associated with development and variable prognosis in PsA.
- Progression to PsA among patients with psoriasis has been reported to occur at a rate of around 2% per year.
- Episodic flares of the disease in addition to chronic, baseline joint inflammation.
- Joint erosion / damage may accrue over time, with the potential for development of functional impairments.



 Patient Information for
Patient Information for