Pustular psoriasis flares can be induced by infection (Trichophyton rubrum, cytomegalovirus, Streptococcus spp, varicella-zoster, and Epstein-Barr virus), a rapid withdrawal of corticosteroids, pregnancy, medications (NSAIDs, lithium, potassium iodine, trazodone, penicillin, interferon, and hydroxychloroquine), and topical irritants such as tar and anthralin. More recently, COVID-19 infection has been shown to trigger a pustular flare in a 12-year-old with prior plaque psoriasis in remission.
While tumor necrosis factor (TNF)-alpha antagonists such as infliximab and adalimumab are used to treat pustular psoriasis, they have also been reported paradoxically to induce it.
There are 3 subtypes of generalized pustular psoriasis:
- von Zumbusch type – Acute onset of generalized erythema and pustules with systemic manifestations including fever, skin tenderness, malaise, arthralgias, headache, and nausea. After several days, the pustules resolve to become confluent, scaling plaques.
- Exanthematic type – Acute onset of small pustules that are triggered by an infection or a drug. This subtype usually lacks systemic symptoms.
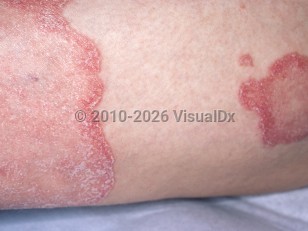
- Annular subtype – Erythematous, annular lesions that have pustules at the advancing edge of a lesion. This subtype is associated with fever, malaise, and other systemic manifestations.
Palmoplantar pustulosis, a localized form of pustular psoriasis, has been shown to occur with increased incidence in smokers and has the lowest association with IL36RN mutations.
Acrodermatitis continua of Hallopeau, in which the distal digits are primarily involved, is a localized form that rarely affects children.
Pustular psoriasis in children often has a more benign course than in adults, and children have a higher rate of spontaneous remission of generalized pustular psoriasis. Pediatric pustular psoriasis may be part of SAPHO syndrome (synovitis, acne, psoriasis / palmoplantar pustulosis, hyperostosis, osteitis).