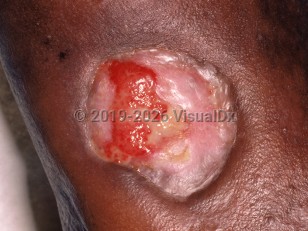
Pyoderma gangrenosum - Anogenital in
See also in: Overview,Cellulitis DDxAlerts and Notices
Important News & Links
Synopsis

PG can take on a number of differing clinical presentations. The 2 most common presentations are a classic ulcerative form, which often involves the lower extremities, and a vesiculobullous form, which is more superficial and tends to occur on the upper extremities, including the hands. This subtype is most commonly seen in patients with an associated lymphoproliferative disorder. Other variants include pustular, vegetative, and peristomal PG. Fever, toxicity, and pain can be associated with the onset of PG. Rarely, PG can involve the eyes. Extracutaneous manifestations may take the form of sterile neutrophilic abscesses, such as in the lungs, heart, gastrointestinal (GI) tract, liver, eyes, central nervous system (CNS), and lymphatic tissue.
Necrotizing neutrophilic dermatosis describes a subset of patients with severe acute febrile neutrophilic dermatosis (Sweet syndrome) or PG who, in addition to their cutaneous disease, develop fever, leukocytosis (or a leukemoid reaction), and features of shock. Skin pain is a prominent symptom. Additionally, soft tissues underlying areas of skin involvement may be affected with neutrophilic infiltrates and necrosis.
Although the exact cause of PG is unknown, neutrophil dysfunction, inflammation, and genetics are all thought to play a role. Additionally, PG has associations with a number of systemic illnesses. In about 50% of cases, there is an association with a systemic disease, such as ulcerative colitis, Crohn disease, arthritis, myeloma, leukemia, monoclonal gammopathy, granulomatosis with polyangiitis, collagen vascular disease, metabolic syndrome, or Behçet disease, among other disorders, including genetic conditions. Surgery by itself can be a precipitating cause (postoperative PG). Levamisole-contaminated cocaine has been associated with PG lesions ranging from vesiculopustules to bullae to larger ulcers; most patients demonstrated positivity for antiphospholipid or anticardiolipin antibodies. PG can be associated with autoinflammatory syndromes (eg, PAPA syndrome [pyogenic arthritis, PG, and acne]; SAPHO syndrome [synovitis, acne, pustulosis, hyperostosis, and osteitis]; and PAPASH syndrome (pyogenic arthritis, PG, acne, and hidradenitis]).
PG can have either an acute or chronic course and results in extensive scarring (which can be cribriform or keloidal with dyspigmentation, especially in patients with darker skin colors). Surgical intervention is a common exacerbating factor because PG demonstrates pathergy, a phenomenon by which skin trauma can lead to worsening disease.
Codes
L88 – Pyoderma gangrenosum
SNOMEDCT:
74578003 – Pyoderma gangrenosum
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:11/26/2023