Rickettsia australis, transmitted by the Ixodes holocyclus, Ixodes tasmani, and Ixodes cornuatus ticks, is a member of the spotted-fever group of Rickettsiae. It causes Queensland tick typhus (QTT), which is only endemic to eastern Australia. It has been reported in both Australians and travelers to eastern Australia.
Patients develop a febrile syndrome with headache and myalgias 1-11 days (mean 5 days) after a tick bite. A diffuse rash follows accompanied by an eschar at the site of the tick bite in one-half to two-thirds of cases. Occasionally, QTT may be "spotless." Lymphadenopathy adjacent to the bite may be present 50%-75% of the time. Hepatomegaly and splenomegaly may be observed as well. Laboratory abnormalities include thrombocytopenia, hyponatremia, renal insufficiency, and transaminitis. At least one fatality has been reported. Complications such as renal failure, pneumonia, and purpura fulminans may rarely occur.
Males are more often infected than females, more patients are affected in the winter and spring months, and up to 90% of patients may give a history of a tick bite.
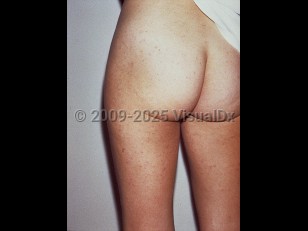
Queensland tick typhus
Alerts and Notices
Important News & Links
Synopsis

Codes
ICD10CM:
A77.3 – Spotted fever due to Rickettsia australis
SNOMEDCT:
68981009 – Queensland tick typhus
A77.3 – Spotted fever due to Rickettsia australis
SNOMEDCT:
68981009 – Queensland tick typhus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:09/06/2017
Queensland tick typhus