Radiation-induced skin reactions can present instantaneously following radiation exposure or decades later. There is no increased predilection for radiation injuries by sex. The predominance of radiation dermatitis in males reflects their higher incidence of coronary artery disease and subsequent increased use of fluoroscopic procedures for therapeutic purposes.
The pathophysiology of radiation dermatitis is complex and multifactorial. It occurs due to immediate damage to skin cells (eg, basal keratinocytes, functional stem cells, melanocytes), oxidative stress, endothelial cell changes, inflammation, cytokine response, and epidermal cell apoptosis and necrosis. Cells in both the epidermis and the dermis are affected. Acute injuries primarily present in the epidermis, whereas chronic or late effects, such as skin fibrosis, primarily involve long-term dysfunction cells in the dermis.
Radiation recall is a well-documented, late acute inflammatory reaction that occurs at sites of previous radiation therapy after administration of antineoplastic agents.
Acute Radiation Dermatitis
Acute radiation dermatitis is common, occurring in up to 90% of individuals receiving radiotherapy. The skin reaction presents within 90 days of radiation exposure. Lesions generally present in a geometric configuration at the irradiated site. Skin changes can include faint erythema, dry desquamation, moist desquamation (macerated scale), necrosis, and ulceration. Pruritus, edema, pigmentary changes, and pain are the most common symptoms associated with acute radiation dermatitis.
The Radiation Therapy Oncology Group (RTOG) and the National Cancer Institute (NCI) have similar criteria for the classification of acute radiation dermatitis:
- Grade 0 – No changes seen.
- Grade 1 – Faint erythema or dry desquamation; common symptoms include pruritus, hair loss, and decreased sweating.
- Grade 2 – Moderate to brisk (bright) erythema or patchy, moist desquamation confined to skin folds and creases. Moderate edema.
- Grade 3 – Confluent, moist desquamation that is not confined to the skin folds. Pitting edema. Bleeding induced by minor trauma or abrasion.
- Grade 4 – Life-threatening consequences. Skin necrosis or ulceration of full thickness dermis. Hemorrhage or spontaneous bleeding from involved site. Skin graft indicated.
- Grade 5 – Death, an extremely rare event due to nuclear / radiation exposure alone.
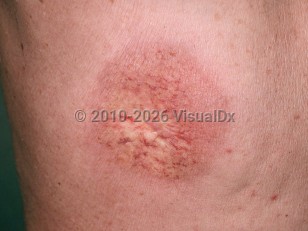
The chronic form usually occurs months (over 90 days) to years after radiation exposure greater than 45 Gy, but onset may occur from 15 days to decades after the beginning of the exposure.
Chronic radiation dermatitis is more likely to occur in individuals with unprotected sun exposure, a larger dose per fraction delivered (> 4 Gy), a larger total dose (> 50 Gy), and with radiation exposure of large body surface areas. Skin changes include telangiectasias, dermal atrophy, fibrosis, necrosis, chronic ulcers, and secondary skin cancers.
Chronic radiation dermatitis is caused by an imbalance of proinflammation and profibrotic cytokines, which can last for years. Tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), and interleukin-1 (IL-1) are responsible for persistent inflammation, whereas tumor growth factor-beta (TGF-β) and platelet-derived growth factor (PDGF) promote fibrosis and telangiectasias. Long-lasting impairment of the skin's ability to heal can be due to compromised cellular dysfunction. Fibroblasts and other skin cells may be permanently altered, leading to atrophy and fibrosis.
To date, no direct connection has been established between experiencing acute radiation dermatitis and developing chronic effects.
Risk Factors for Radiation Dermatitis
- Poor nutritional status
- Obesity
- Chronic sun exposure
- Smoking and/or chewing tobacco
- Senescence
- Problems with skin integrity
- Overlapping skin folds
- High total radiation dose
- Large irradiated volume (large radiation field size)
- High radiation per fractional dose (>3 Gy per dose)
- Irradiation of the anterior neck, extremities, chest, breasts, abdomen, face, or hair follicles on the scalp
- Use of a bolus during radiotherapy that increases radiation dose to the skin
- Prolonged or multiple procedures requiring radiation exposure
- Concurrent chemotherapy and targeted anticancer therapies, such as EGFRI with radiotherapy, increases the risk of severe reactions.
- Some connective tissue diseases (ie, systemic lupus erythematosus, scleroderma, and possibly rheumatoid arthritis)
- Diseases with reduced cellular DNA capability, such as hereditary nevoid basal cell carcinoma (BCC)
- Diseases involving chromosomal breakage syndromes, like Fanconi anemia and Bloom syndrome
- Homozygosity for the ataxia-telangiectasia gene (ATM)
- HIV disease
- Vasculopathies such as diabetes and hypertension
- Radiosensitizing drugs (eg, paclitaxel or docetaxel) given before or up to 7 days after radiation therapy