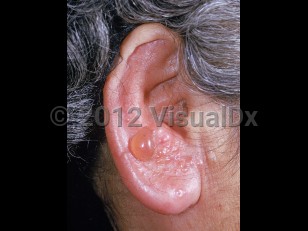
Ramsay-Hunt syndrome
Alerts and Notices
Important News & Links
Synopsis

Ramsay-Hunt syndrome generally starts with a 1- to 3-day prodrome of otalgia and ipsilateral facial paralysis followed by development of herpetic vesicles on the face just anterior to the tragus and on various parts of the ear, including the auricle, external ear canal, and tympanic membrane. However, some patients may experience vesicle formation preceding development of ipsilateral otalgia and facial paralysis. Vesicles may also appear on the mouth and anterior two-thirds of the tongue. Evolution of disease may differ between age groups; in children, the vesicles may appear several days after the facial paralysis. Over the course of a week, the vesicles become pustules and then ulcerate to form crusts.
The lesions heal within weeks and may result in scarring. However, facial paralysis may be chronic unless antiviral with or without simultaneous corticosteroid treatment is initiated within 72 hours of disease presentation. Other symptoms and signs can include tinnitus, hearing loss, vertigo, hyperacusis, nystagmus, nausea, vomiting, taste impairment, lesions of the oral mucosa, dry mouth, and dry eyes. Cerebrovascular accidents have been associated with zoster.
Diagnosis is primarily clinical and is based on a combination of facial palsy, otalgia, and vesicles on the pinna or oral mucosa. Ramsay-Hunt syndrome is the second most common cause of nontraumatic peripheral facial paralysis, behind Bell palsy (idiopathic facial palsy), and tends to cause more severe paralysis. It has a worse prognosis for facial nerve recovery than Bell palsy, especially in children.
Only 10% of patients with complete facial paralysis are totally cured. Prognosis for associated hearing loss is very good, with only around 5% of patients having residual impairment.
Related topics: herpes zoster, varicella
Codes
B02.21 – Postherpetic geniculate ganglionitis
SNOMEDCT:
21954000 – Herpes zoster auricularis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:02/23/2022