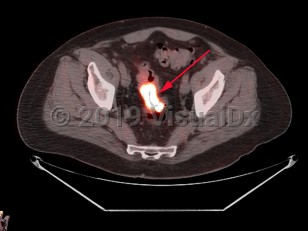
Rectal carcinoma
Alerts and Notices
Important News & Links
Synopsis

The majority of rectal cancers are adenocarcinomas, which arise from a background of adenomatous dysplasia. The risk factors for developing CRC are numerous. There are adenomatous polyposis syndromes such as familial adenomatous polyposis, hereditary nonpolyposis colorectal cancer, and MUTYH-associated polyposis (MAP) that significantly increase a person's risk of developing CRC. Smoking is also a risk factor. A personal or family history of sporadic CRCs or adenomatous polyps is also concerning. Other inflammatory conditions such as inflammatory bowel disease (especially ulcerative colitis) are risk factors for the development of CRC.
CRC rates are highest among African Americans compared with other populations in the United States. Patients with a low socioeconomic status have also been shown to have an increased risk of developing CRC. The incidence of rectal cancer is higher among men than women. Overall, the incidence of colorectal cancer in older patients, particularly those aged 65 years and older, is declining, likely due to a combination of screening and changes in risk factors (eg, decreased smoking). But for patients aged younger than 55 years, the incidence of colorectal cancer has been rising.
Patients with cancers of the rectum or rectosigmoid region often present with hematochezia, tenesmus, and narrowing of the stool. Anemia is uncommon at presentation.
The most common sites of metastasis of colorectal adenocarcinoma are the liver and lungs; rarely, metastatic oral lesions occur.
The US Preventive Services Task Force (USPSTF) recommends screening for CRC using noninvasive blood tests, sigmoidoscopy, or colonoscopy in adults, beginning at age 50 years and continuing until age 75 years. Earlier screening is appropriate for patients with a family history of CRC. Some experts recommend screening everyone beginning at age 45 years.
Codes
C20 – Malignant neoplasm of rectum
SNOMEDCT:
254582000 – Adenocarcinoma of rectum
93984006 – Primary malignant neoplasm of rectum
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/05/2023