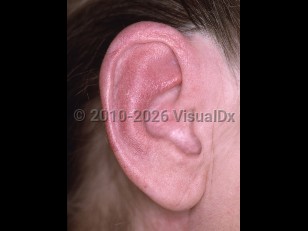
Relapsing polychondritis
See also in: Cellulitis DDx,External and Internal EyeAlerts and Notices
Important News & Links
Synopsis

Relapsing polychondritis is an autoimmune multisystemic condition affecting cartilaginous structures such as the ears, nose, eyes, joints, larynx, and tracheobronchial tree.
The course and clinical aspects of relapsing polychondritis vary significantly across patients, and early manifestations of disease are often extremely subtle and go unrecognized. Signs and symptoms of relapsing polychondritis include auricular, nasal, costal, and laryngotracheobronchial chondritis; arthropathy; ocular inflammation (eg, episcleritis); audiovestibular damage; cardiovascular disease (aortitis, aortic aneurysm, or regurgitation); cutaneous vasculitis; central nervous system (CNS) disturbances (eg, cranial neuropathies, seizures); and renal involvement.
Auricular chondritis is the most common clinical feature, and nasal chondritis is present in around 25% of patients at diagnosis. Nasal pain, hoarseness, throat pain, and difficulty talking are common presenting symptoms.
Ocular manifestations of relapsing polychondritis are frequent (59% of cases) and can affect almost any part of the eye, which makes diagnosis based on ocular findings alone extremely difficult. These findings include conjunctivitis, keratitis, scleritis, episcleritis, uveitis, retinopathy (cotton wool spots and intraretinal hemorrhages), and in those with associated vasculitis, optic nerve involvement and cranial nerve palsies.
Flares are accompanied by fever, asthenia, weight loss, and sometimes liver or lymph node enlargement.
Relapsing polychondritis is frequently associated with other autoimmune connective tissue disorders, vasculitis, and myelodysplastic syndromes. Complications include saddle-nose deformity / joint deformity, vertigo, tinnitus, pulmonary infection, laryngotracheobronchial stricture, scleritis or iritis, epiglottitis, blindness, valve regurgitation, aortic dissection, renal failure, and death. Relapsing polychondritis is more common in the White population and between the ages of 40 and 60 years. The disease equally affects male and female patients.
The course and clinical aspects of relapsing polychondritis vary significantly across patients, and early manifestations of disease are often extremely subtle and go unrecognized. Signs and symptoms of relapsing polychondritis include auricular, nasal, costal, and laryngotracheobronchial chondritis; arthropathy; ocular inflammation (eg, episcleritis); audiovestibular damage; cardiovascular disease (aortitis, aortic aneurysm, or regurgitation); cutaneous vasculitis; central nervous system (CNS) disturbances (eg, cranial neuropathies, seizures); and renal involvement.
Auricular chondritis is the most common clinical feature, and nasal chondritis is present in around 25% of patients at diagnosis. Nasal pain, hoarseness, throat pain, and difficulty talking are common presenting symptoms.
Ocular manifestations of relapsing polychondritis are frequent (59% of cases) and can affect almost any part of the eye, which makes diagnosis based on ocular findings alone extremely difficult. These findings include conjunctivitis, keratitis, scleritis, episcleritis, uveitis, retinopathy (cotton wool spots and intraretinal hemorrhages), and in those with associated vasculitis, optic nerve involvement and cranial nerve palsies.
Flares are accompanied by fever, asthenia, weight loss, and sometimes liver or lymph node enlargement.
Relapsing polychondritis is frequently associated with other autoimmune connective tissue disorders, vasculitis, and myelodysplastic syndromes. Complications include saddle-nose deformity / joint deformity, vertigo, tinnitus, pulmonary infection, laryngotracheobronchial stricture, scleritis or iritis, epiglottitis, blindness, valve regurgitation, aortic dissection, renal failure, and death. Relapsing polychondritis is more common in the White population and between the ages of 40 and 60 years. The disease equally affects male and female patients.
Codes
ICD10CM:
M94.1 – Relapsing polychondritis
SNOMEDCT:
72275000 – Relapsing polychondritis
M94.1 – Relapsing polychondritis
SNOMEDCT:
72275000 – Relapsing polychondritis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:07/26/2021
Last Updated:08/04/2021
Last Updated:08/04/2021
Relapsing polychondritis
See also in: Cellulitis DDx,External and Internal Eye