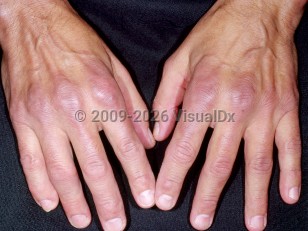
Rheumatoid arthritis
Alerts and Notices
Important News & Links
Synopsis
Onset is usually subtle, with morning stiffness for over 30 minutes, and commonly associated with fatigue. Untreated, RA causes joint destruction with resultant disability and even increased mortality. With the development of newer medications, early and aggressive therapy can afford people with RA preserved function and improved quality of life.
RA is characterized by inflammation in the synovial membrane caused by infiltration of T cells, B cells, and monocytes, resulting in inflammation in the joint synovium. This inflammatory state leads to articular cartilage loss and bony erosion, resulting in irreversible damage and functional impairment. The onset of disease is insidious, most typically presenting with symmetric polyarthritis described as pain, swelling, and inflammation of joints leading to stiffness after a period of inactivity. Some patients present with constitutional symptoms including malaise, fatigue, and depressed mood as well as low-grade fevers and weight loss. Patients may develop anemia of chronic disease.
Classically, this symmetrically distributed polyarthritis affects the small joints of the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and metatarsophalangeal (MTP) joints early in disease. Other synovial joints may be involved, including the elbows, shoulders, ankles, and knees. Of note, the C1-C2 joints of the spine and temporomandibular, sternoclavicular, or cricoarytenoid joints may be involved. Less common initial presentations include a monarticular or oligoarticular arthritis.
RA is labeled "seropositive" when rheumatoid factor (RF) and/or anti-citrullinated protein antibodies (ACPAs) are present. Seropositive disease tends to be more severe and associated with increased risk of systemic involvement. Rheumatoid nodules occur in up to 20% of RA patients and more frequently among patients with seropositive disease.
Initial evaluation of the patient presenting with joint pain should focus on determining whether the presenting arthritis pain is inflammatory vs. noninflammatory in nature. For example, inflammatory joint symptoms include a joint stiffness that occurs after inactivity – including in the morning after waking (> 30 minutes of stiffness) – and improves with activity. Signs of inflammation such as redness, swelling, and warmth should prompt consideration of inflammatory and infectious arthritides.
Codes
M06.9 – Rheumatoid arthritis, unspecified
SNOMEDCT:
69896004 – Rheumatoid arthritis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/08/2023
 Patient Information for Rheumatoid arthritis
Patient Information for Rheumatoid arthritis - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient