Scabies is designated as one of the neglected tropical diseases (NTDs) by the World Health Organization (WHO) because of the disease burden and its complications, particularly in areas with limited health care access, and its potential public health control strategies. Factors that contribute to the persistence and spread of scabies are overcrowding, delays in diagnosis, and poor public health awareness. Outbreaks in health care facilities can result in dozens of patients and staff becoming infected. Epidemiologically, scabies affects children much more commonly than adults, and the chance of bacterial superinfection in children is high.
In a typical infestation, there are 10-20 mites. The mite burrows into the stratum corneum of the epidermis, and most patients mount an intense hypersensitivity reaction to the mites, eggs, and/or feces. This results in a widespread and highly pruritic eruption that can result in disruption of the cutaneous barrier and superinfection. In those who are acquiring scabies for the first time, the hypersensitivity reaction usually develops 2-6 weeks after initial infestation, but in those with previous history of infestation, the itching may start in 24-72 hours. Without medical treatment, the condition persists because the mites lay eggs, causing continued infestation.
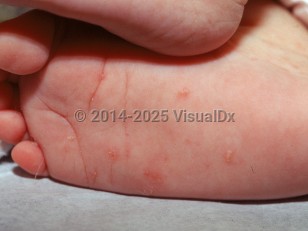
The most common clinical manifestation of scabies in infants is the development of pustules, vesicles, and crusting. The palms and soles, fingers, face, and scalp are most heavily involved. Secondary impetigo and eczematization are common. The primary symptom of infestation is pruritus, and in young infants who have not developed a coordinated itch response, this may manifest as rubbing the head against a caregiver, irritability, insomnia, poor feeding, and failure to thrive.
Clinically, scabies infestation manifests in 2 ways: classic scabies or crusted scabies (previously called Norwegian scabies).
- Classic scabies in children presents with pruritic papules affecting the flexural areas, including the axillary folds, wrists, and dorsal ankles; the interdigital web spaces of the hands and feet; the anogenital area; and the truncal area, especially around the nipples and periumbilical area. The papules are accompanied by itch, which is classically worse at night, especially just after getting into bed. Nodular scabies, a clinical variant of classic scabies, is less common in children than in adults. It is considered a hypersensitivity reaction to the mite and manifests with erythematous nodules.
- The crusted variant of scabies is most common in individuals who are malnourished and/or immunocompromised. It presents with widespread scaly, crusted, or hyperkeratotic papules and plaques. Scales may have a powdery texture. Pruritus may be severe but is usually minimal or absent. Nail dystrophy can be present. It is extremely contagious due to the high mite burden; there may be up to a million mites on a single individual.



 Patient Information for
Patient Information for