Schistosomiasis
Alerts and Notices
Important News & Links
Synopsis

Schistosomiasis (also known as bilharziasis) is an acute and chronic parasitic disease caused by infection with a trematode of the genus Schistosoma. Schistosomiasis is acquired through the skin during exposure to freshwater infested with cercariae, eg, while wading or walking through fresh water in ponds, lakes, and rivers; while swimming or bathing; or while washing clothes in contaminated water.
Schistosomiasis is endemic in many parts of Africa, South America, the Caribbean, China, Southeast Asia, and the Middle East. Infection is more prevalent in those living in tropical and subtropical areas lacking adequate sanitation. Travelers to endemic regions who are exposed to contaminated water are also at risk. Over 200 million people are infected worldwide.
After development in the intermediate aquatic snail host, parasites are released into fresh water as cercariae. They penetrate the skin and become schistosomula. They then migrate to the liver and become adult trematodes (1-3 cm long). Mating adults migrate to venules of the genitourinary tract (in the case of Schistosoma haematobium) and gastrointestinal tract (in the case of Schistosoma mansoni, Schistosoma japonicum, Schistosoma intercalatum, and Schistosoma mekongi) where they produce eggs that are shed in the urine and feces, respectively. After infected individuals urinate or defecate in the water, eggs hatch, reinfecting the snails.
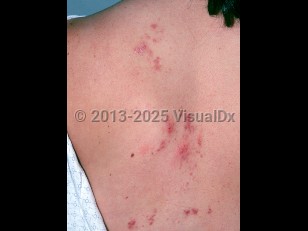
Within a few days after exposure, an individual may develop a rash that then clears. Acute schistosomiasis may be asymptomatic or it may cause a systemic allergic reaction, especially in individuals who are visiting endemic areas on first exposure. It occurs approximately 1 month after exposure when adult parasites begin laying eggs. Urticaria, fever, sweats, chills, cough, and headache are accompanied by lymphadenopathy and hepatosplenomegaly. Respiratory and gastrointestinal symptoms may also occur. This syndrome is known as Katayama fever. It is usually seen with S japonicum infection, but more recently cases from S mansoni have also been recognized.
Without treatment, chronic disease will develop and may persist for years. Complications of chronic schistosomiasis occur as a result of the granulomatous response to eggs in affected tissues and subsequent fibrosis. Liver, intestine, spleen, lungs, and bladder can be involved. Chronic bladder involvement leads to an increased risk of bladder cancer. Rarely, there may be central nervous system (CNS) involvement, causing myelopathy, seizures, or paralysis.
In girls and women, S haematobium eggs in the cervix, vagina, and vulva can cause development of "rubbery" or yellow, sandy patches, which may bleed; genital pruritus; abnormal discharge; dyspareunia; and stress incontinence. Infertility can be a long-term complication. While genital schistosomiasis is one of the most common gynecologic conditions in Africa, it is often confused with sexually transmitted infections and, because of damage to the hymen, can lead to accusations of sexual promiscuity. The condition often leads to depression.
Age-related demographics:
All ages and sexes are susceptible. However, the prevalence and severity is highest in children and slowly declines with age.
It has been shown that women and men with lower urinary schistosomiasis have a significantly increased risk of acquiring HIV and subsequently transmitting it to their sexual partners.
Schistosomiasis is endemic in many parts of Africa, South America, the Caribbean, China, Southeast Asia, and the Middle East. Infection is more prevalent in those living in tropical and subtropical areas lacking adequate sanitation. Travelers to endemic regions who are exposed to contaminated water are also at risk. Over 200 million people are infected worldwide.
After development in the intermediate aquatic snail host, parasites are released into fresh water as cercariae. They penetrate the skin and become schistosomula. They then migrate to the liver and become adult trematodes (1-3 cm long). Mating adults migrate to venules of the genitourinary tract (in the case of Schistosoma haematobium) and gastrointestinal tract (in the case of Schistosoma mansoni, Schistosoma japonicum, Schistosoma intercalatum, and Schistosoma mekongi) where they produce eggs that are shed in the urine and feces, respectively. After infected individuals urinate or defecate in the water, eggs hatch, reinfecting the snails.
Within a few days after exposure, an individual may develop a rash that then clears. Acute schistosomiasis may be asymptomatic or it may cause a systemic allergic reaction, especially in individuals who are visiting endemic areas on first exposure. It occurs approximately 1 month after exposure when adult parasites begin laying eggs. Urticaria, fever, sweats, chills, cough, and headache are accompanied by lymphadenopathy and hepatosplenomegaly. Respiratory and gastrointestinal symptoms may also occur. This syndrome is known as Katayama fever. It is usually seen with S japonicum infection, but more recently cases from S mansoni have also been recognized.
Without treatment, chronic disease will develop and may persist for years. Complications of chronic schistosomiasis occur as a result of the granulomatous response to eggs in affected tissues and subsequent fibrosis. Liver, intestine, spleen, lungs, and bladder can be involved. Chronic bladder involvement leads to an increased risk of bladder cancer. Rarely, there may be central nervous system (CNS) involvement, causing myelopathy, seizures, or paralysis.
In girls and women, S haematobium eggs in the cervix, vagina, and vulva can cause development of "rubbery" or yellow, sandy patches, which may bleed; genital pruritus; abnormal discharge; dyspareunia; and stress incontinence. Infertility can be a long-term complication. While genital schistosomiasis is one of the most common gynecologic conditions in Africa, it is often confused with sexually transmitted infections and, because of damage to the hymen, can lead to accusations of sexual promiscuity. The condition often leads to depression.
Age-related demographics:
All ages and sexes are susceptible. However, the prevalence and severity is highest in children and slowly declines with age.
It has been shown that women and men with lower urinary schistosomiasis have a significantly increased risk of acquiring HIV and subsequently transmitting it to their sexual partners.
Codes
ICD10CM:
B65.9 – Schistosomiasis, unspecified
SNOMEDCT:
10087007 – Schistosomiasis
B65.9 – Schistosomiasis, unspecified
SNOMEDCT:
10087007 – Schistosomiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:01/21/2018
Last Updated:01/12/2020
Last Updated:01/12/2020