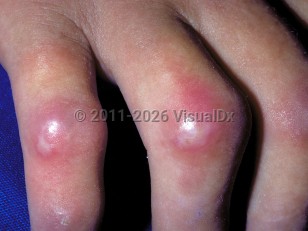
Scleroderma, or progressive systemic sclerosis, is an autoimmune connective tissue disease that involves sclerotic changes of the skin and may involve internal organs. While the etiology remains unknown, the disease is characterized by autoantibody production, collagen deposition, and vascular dysfunction. The disease is observed in all ages and is slightly more common in Black individuals and 3-4 times more common in women. The age of onset is usually between 30 and 50 years.
Scleroderma can affect the connective tissue of any organ, including the skin, gastrointestinal tract, lungs, kidneys, joints, muscles, heart, and blood vessels. Pulmonary disease is the leading cause of mortality. Additional common clinical features include esophageal dysfunction, primarily characterized by dysmotility, arthralgias, and Raynaud phenomenon. Less common manifestations include hypertensive renal crisis, pulmonary hypertension and interstitial lung disease, and cardiomyopathy.
The 3 major clinical subsets of scleroderma are limited cutaneous systemic sclerosis, diffuse cutaneous systemic sclerosis, and systemic sclerosis sine scleroderma.
CREST syndrome (calcinosis cutis, Raynaud phenomenon, esophageal dysfunction, sclerodactyly, and telangiectasia) refers to a subset of patients with limited scleroderma.
The systemic sclerosis overlap syndrome is characterized by features of one of the scleroderma subsets with those of another autoimmune disease (eg, lupus erythematosus, dermatomyositis, Sjögren syndrome, and/or rheumatoid arthritis).
Many nail findings are seen in scleroderma. Examination of the proximal nail fold reveals capillary enlargement and loss of some capillaries in most scleroderma patients. Other common nail changes include the following:
- Trachyonychia (roughness; "sandpaper nails")
- Scleronychia (hardened, inelastic, opaque)
- Brachyonychia (short nail, with width exceeding length; "racquet nail")
- Splinter hemorrhages
- Nail thickening
- Parrot beaking (overcurvature of the fingernail free edge; hooked nail deformity)
- Pterygium inversus (distal expansion of the hyponychium, which anchors to the undersurface of the nail plate, ultimately resulting in the obliteration of the distal nail groove)
- Cuticle changes
Related topic: drug-induced sclerodermoid reactions



 Patient Information for
Patient Information for