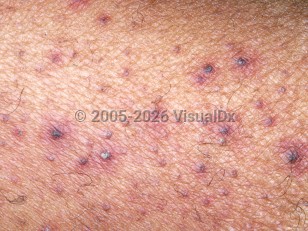
Scurvy in Adult
See also in: Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Scurvy is an acquired condition caused by a prolonged deficiency of vitamin C (L-ascorbic acid). Vitamin C is a water-soluble, essential vitamin that can only be obtained through the diet. It is an essential cofactor in the cross-linking and stabilization of collagen; thus, deficiency of this nutrient causes impaired collagen synthesis, leading to poor wound healing, capillary fragility, and bone abnormalities (eg, osteoporosis, fractures, bone marrow edema, demineralization, intraosseous hemorrhage). Symptoms can develop after 8-12 weeks of insufficient vitamin C intake.
Scurvy is a relatively rare diagnosis in the developed world. Pathognomonic clinical findings of scurvy include gingival bleeding and perifollicular petechiae with corkscrew hairs. Other common features include vascular fragility, manifesting as purpura, petechiae, ecchymoses, and gastrointestinal bleeding. Spontaneous hemorrhage into muscles, soft tissues, and joints can cause painful hematomas and hemarthroses. Symptoms include fatigue, weakness, muscle cramping, and malaise as well as cognitive impairment and mood disturbances. Up to 80% of patients with scurvy present with (mostly mild) anemia.
Risk factors for developing scurvy include alcohol use, low socioeconomic status, restrictive diets or dietary fads, obesity, psychiatric disease, and malabsorption due to gastrointestinal disease. Additionally, older adults, especially those in social isolation; patients on dialysis; and individuals with increased metabolic requirements (such as pregnant or lactating individuals and patients with severe infections) are at increased risk. People who chronically abuse alcohol are particularly susceptible to scurvy not only due to poor dietary intake but also decreased ascorbic acid absorption.
Scurvy is a relatively rare diagnosis in the developed world. Pathognomonic clinical findings of scurvy include gingival bleeding and perifollicular petechiae with corkscrew hairs. Other common features include vascular fragility, manifesting as purpura, petechiae, ecchymoses, and gastrointestinal bleeding. Spontaneous hemorrhage into muscles, soft tissues, and joints can cause painful hematomas and hemarthroses. Symptoms include fatigue, weakness, muscle cramping, and malaise as well as cognitive impairment and mood disturbances. Up to 80% of patients with scurvy present with (mostly mild) anemia.
Risk factors for developing scurvy include alcohol use, low socioeconomic status, restrictive diets or dietary fads, obesity, psychiatric disease, and malabsorption due to gastrointestinal disease. Additionally, older adults, especially those in social isolation; patients on dialysis; and individuals with increased metabolic requirements (such as pregnant or lactating individuals and patients with severe infections) are at increased risk. People who chronically abuse alcohol are particularly susceptible to scurvy not only due to poor dietary intake but also decreased ascorbic acid absorption.
Codes
ICD10CM:
E54 – Ascorbic acid deficiency
SNOMEDCT:
76169001 – Scurvy
E54 – Ascorbic acid deficiency
SNOMEDCT:
76169001 – Scurvy
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/03/2017
Last Updated:09/15/2025
Last Updated:09/15/2025
Scurvy in Adult
See also in: Oral Mucosal Lesion