Syphilis (also known as lues) is a sexually transmitted infection (STI) caused by the spirochete Treponema pallidum. Treponema pallidum is transmitted from person to person through contact with infectious lesions during vaginal, anal, or oral sexual activity, especially when there is disrupted epithelium, such as from minor trauma. Secondary syphilis is the second stage of the infection.
The natural history of syphilis is as follows:
Primary stage:
- Primary lesion develops 10-90 days (average of 21 days) after direct inoculation.
- Primary lesion is typically a painless, asymptomatic papule, followed by a painless ulcer (chancre) and regional lymphadenopathy.
- Chancre lasts 3-6 weeks and heals spontaneously.
- Locations for chancres may include the vagina, cervix, penis, anus, rectum, lips, and inside of the mouth.
- Secondary syphilis is caused by hematogenous dissemination of bacteria.
- A wide range of clinical manifestations, dominated by prodromal symptoms and mucocutaneous manifestations 3-10 weeks after the appearance of the primary chancre.
- Prodromal symptoms and signs – Malaise, appetite loss, fever, headache, stiff neck, myalgias, pharyngitis, and flu-like symptoms. Generalized lymphadenopathy is typically present.
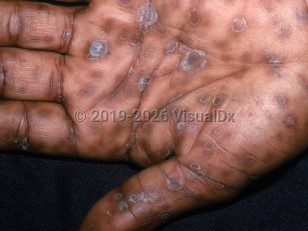
- Cutaneous manifestations – Generalized nonpruritic papulosquamous eruption typically including the palms and soles, with pink, violaceous, or copper-colored papules, each with a collarette of scale. Patchy alopecia of the scalp is also observed in secondary syphilis.
- Mucosal lesions – Mucous patches and "snail-track" ulcers in the mouth, and condyloma lata (gray, flat, moist papules and plaques) may be seen in moist anogenital locations or, more rarely, in the folds. They are teeming with spirochetes and are, therefore, extremely infectious.
- Rheumatologic manifestations – Inflammatory arthritis, tenosynovitis, and dactylitis (especially of the hands and wrists) are reported to occur in a minority of patients.
- Gastric ulcers may occur.
- Ocular symptoms may include lacrimation, photophobia, and red, painful eyes.
- Malignant syphilis (lues maligna) is a rare, noduloulcerative manifestation of secondary syphilis. A generalized eruption of papules and nodules progresses to painful, necrotic ulcers that may have overlying thick or rupioid (darkly colored and conical) crusts. Constitutional symptoms and generalized lymphadenopathy are usually seen. Most contemporary cases of malignant syphilis have been reported in the setting of underlying HIV infection.
- Mucocutaneous manifestations and prodromal symptoms last 3-12 weeks and resolve spontaneously.
- If left untreated, up to 25% of patients will relapse within the first 2 years.
- May appear months to years after secondary syphilis resolves and can involve the central nervous system, heart, bones, and skin.
Immunocompromised patient considerations: HIV infection can alter the clinical presentation of syphilis. Manifestations include multiple chancres, atypical cutaneous eruptions, increased severity of organ involvement (such as hepatitis and glomerulonephritis), and rapidly developing arteritis and neurosyphilis. Neurosyphilis can occur at any stage of syphilis.
Other related topics: early congenital syphilis, late congenital syphilis, ocular syphilis



 Patient Information for
Patient Information for