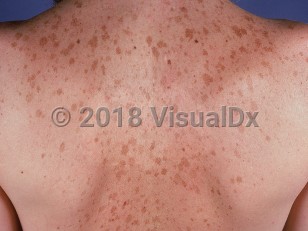
Solar lentigo
See also in: Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Solar lentigo (a type of lentigo also known as a senile lentigo, age spot, or liver spot) is a benign pigmented macule appearing on individuals with light skin that is related to ultraviolet radiation (UVR) exposure, typically from the sun. It must be distinguished from lentigo maligna.
Solar lentigines are believed to be UVR-induced proliferative responses of the epidermal keratinocytes and/or melanocytes, although the exact mechanism of formation is not completely understood. Ultraviolet B (UVB) exposure is thought to increase expression of keratinocyte growth factor, which thereby induces tyrosinase expression and melanin production in melanocytes. This melanin pigment is then transferred to keratinocytes where there is abnormal pigment retention.
Solar lentigines are more common in those with skin phototypes I-III and a history of multiple sunburns. They are present in 90% of individuals over 60 years of age who are of Northern European descent. They may also be seen in younger individuals with extensive UVR exposure and have been observed as early as 5 years of age in children with xeroderma pigmentosum. They are typically located on sun-exposed skin, including the face, upper chest, shoulders, dorsal arms, and hands. Solar lentigines are asymptomatic although they may enlarge, darken, or remain unchanged over time.
A variant is the psoralen ultraviolet A (PUVA)-induced lentigo, which is seen in approximately 50% of patients with at least 6 years of PUVA therapy and may sometimes be distinguished by large, somewhat atypical melanocytes on histopathology. These may be present on any body surface exposed to PUVA, including the genitalia.
Solar lentigines are believed to be UVR-induced proliferative responses of the epidermal keratinocytes and/or melanocytes, although the exact mechanism of formation is not completely understood. Ultraviolet B (UVB) exposure is thought to increase expression of keratinocyte growth factor, which thereby induces tyrosinase expression and melanin production in melanocytes. This melanin pigment is then transferred to keratinocytes where there is abnormal pigment retention.
Solar lentigines are more common in those with skin phototypes I-III and a history of multiple sunburns. They are present in 90% of individuals over 60 years of age who are of Northern European descent. They may also be seen in younger individuals with extensive UVR exposure and have been observed as early as 5 years of age in children with xeroderma pigmentosum. They are typically located on sun-exposed skin, including the face, upper chest, shoulders, dorsal arms, and hands. Solar lentigines are asymptomatic although they may enlarge, darken, or remain unchanged over time.
A variant is the psoralen ultraviolet A (PUVA)-induced lentigo, which is seen in approximately 50% of patients with at least 6 years of PUVA therapy and may sometimes be distinguished by large, somewhat atypical melanocytes on histopathology. These may be present on any body surface exposed to PUVA, including the genitalia.
Codes
ICD10CM:
L81.4 – Other melanin hyperpigmentation
SNOMEDCT:
72100002 – Solar lentigo
L81.4 – Other melanin hyperpigmentation
SNOMEDCT:
72100002 – Solar lentigo
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:01/29/2023
 Patient Information for Solar lentigo
Patient Information for Solar lentigo
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today