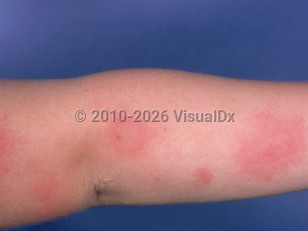
Solar urticaria in Child
Alerts and Notices
Important News & Links
Synopsis

Solar urticaria presents with classic urticarial wheals, erythema, and/or edema limited to sun-exposed areas of the body within minutes of sun exposure. Lesions typically resolve within 1-2 hours after exposure. Regularly sun-exposed areas, such as the face and dorsal hands, may be less sensitive due to the hardening phenomenon. Fixed solar urticaria is a subtype in which lesions occur exclusively in the same localized area of the skin.
Most patients experience accompanying pruritus or a burning sensation, and rarely pain has been described. Systemic symptoms are uncommon but may occur after prolonged exposure of a large body surface area to inciting radiation; symptoms may include headache, nausea, dizziness, wheezing, dyspnea, and syncope. Rarely, severe attacks are associated with anaphylactic shock.
Solar urticaria is caused by immunoglobulin E (IgE)-mediated mast cell degranulation. However, the exact mechanism triggering the degranulation is not known. It is thought to be an IgE-mediated response to a photoinduced allergen. Chlorpromazine, tar, benoxaprofen, and repirinast are known causes of drug-induced solar urticaria.
Solar urticaria typically follows a chronic course. The mean age of onset is 35 years, with less than 4% of patients presenting before age 5. Spontaneous resolution may occur in 15% of patients after 5 years and approximately 25% of patients after 10 years of symptoms. Occasionally, repeat exposure may produce a hardening effect with decreased severity or frequency of symptoms.
Codes
L56.3 – Solar urticaria
SNOMEDCT:
10347006 – Solar urticaria
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:12/13/2020