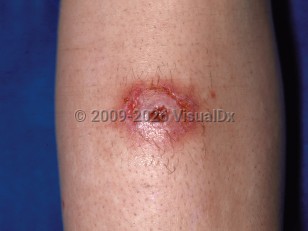
Spider bite in Child
Alerts and Notices
Important News & Links
Synopsis

Spiders are members of the phylum Arthropoda, which includes insects, scorpions, crustaceans, and other similar creatures that have segmented bodies with appendages on each segment. Spiders are invertebrate animals that produce silk and have 8 legs and are wingless. They are found in all habitats except for the open sea. The jaws of spiders have fangs that deliver venom via a small hole at the tips. The venom is primarily used to incapacitate or initiate digestion of prey. Composition, potency, and clinical effects of venom vary among the different spider species. Spiders that hunt typically have more potent venoms than web-spinning spiders (except the widow spiders).
There are over 34,000 named species of spiders in the world. Almost all species are venomous, but only a few dozen can harm humans. Most spiders either do not have an adequate amount of venom to cause harm, the venom is not toxic to humans, or the fangs cannot penetrate human skin. Of the few spiders that are of medical importance, envenomation can cause a range of clinical manifestations from skin lesions to systemic illness and even death. Tarantulas have venom but usually cause illness from their urticating hairs.
Spiders with cytotoxic venoms cause local tissue injury. The bite is often painless at first, and then symptoms of pain and swelling at the bite site develop minutes to hours later. Some lesions resolve spontaneously while others go on to ulcerate and, at times, develop significant necrosis requiring medical attention. The recluse spiders (eg, Loxosceles reclusa and Loxosceles laeta) have cytotoxic venoms.
Bites from spiders with neurotoxic venoms affect the neuromuscular junctions, causing systemic symptoms from cholinergic and catecholamine excess. Often, the bite is very painful, and systemic symptoms include hypertension, tachycardia, palpitations, diaphoresis, anxiety, shortness of breath, hyperthermia or hypothermia, excessive salivation, nausea, vomiting, and severe pain. The widow spiders, Latrodectus species, have neurotoxic venoms.
The severity of a spider bite depends on the type and amount of venom injected, the site of the bite, and the health and age of the patient. Classically, spider bites are asymptomatic in children. However, when symptomatic (because of the large quantity of venom per kilogram), children are more likely to have systemic reactions than adults.
While there are no spiders that can be described as "truly deadly" (ie, lack of treatment can be expected to result in death), spiders of medical importance include:
Widow spiders
Spiders of the Latrodectus genus are found worldwide and have neurotoxic venoms, with alpha-latrotoxin as the major component that can cause severe systemic symptoms from massive neurotransmitter release. The bite is sharp and painful, and fang marks, diaphoresis, and a halo-like lesion may be seen.
In children, most black widow spider bites become asymptomatic within 48 hours. In more severe black widow bites, however, children can also experience diaphoresis, emesis, and abdominal pain. The abdominal pain can often be confused with peritonitis, and thus a careful history is necessary. Of note, those with peritonitis have pain with movement, while those with a spider bite are hypertensive and agitated, and move frequently to find a comfortable position.
Special Considerations in Infants:
Infants bitten by black widow spiders may present differently from toddlers or children, with non-specific signs and symptoms including poor feeding, irritability, and occasionally full body erythema. Often there is a history of sleeping in a bed that was stored in an outdoor shed.
False black widow spiders
Steatoda spiders are found worldwide and have venom capable of producing symptoms similar to Latrodectus but milder.
Recluse spiders
Spiders of the Loxosceles genus are found worldwide in temperate and tropical regions. Envenomation can cause local necrosis and, rarely, severe systemic symptoms. The brown recluse spider is regularly and erroneously blamed as the cause of necrotic lesions throughout the United States, although this spider is only endemic to the southeastern states.
In severe cases of Loxosceles envenomation in children, patients may present with hemolytic anemia, rhabdomyolysis, acute renal failure, or cellulitis. The most common admission diagnoses for spider bites include hemolytic anemia, cellulitis, and acute renal failure.
Hobo spiders
In the Pacific Northwest, the hobo spider (Tegenaria agrestis) is often blamed as the cause of necrotic skin lesions. However, there is only one documented case of hobo spider envenomation causing dermonecrosis. Other presumed cases are based on anecdotal reports and circumstantial evidence.
Yellow sac spiders
Yellow sac spiders, Cheiracanthium species, are found in North America, Europe, Africa, Asia, Australia, and the Pacific Islands. Envenomation is believed to cause dermonecrosis, but like the hobo spider, T. agrestis, and wolf spider, Lycosa species, the data do not support this association.
Wolf spiders
The wolf spiders, Lycosa species, are common spiders found worldwide. The bite from a wolf spider is typically transiently painful, generally lasting only several minutes. A local reaction might be evident; systemic symptoms are rare. There are no data to support the belief that envenomation causes necrotic lesions.
Banana spiders
Phoneutria species, of Central and South America, have extremely potent venom that is neurotoxic and can be lethal.
Australian funnel-web spiders
Atrax/Hadronyche species in Australia include the most dangerous spider, the Sydney funnel-web spider (Atrax robustus). The venom of this spider is neurotoxic, capable of producing severe pain at the bite site and systemic symptoms that can, rarely, be fatal within minutes.
Six-eyed crab spiders
Spiders of the Sicarius genus are found in Africa and South America and are considered to be extremely venomous but, fortunately, live in remote areas. Their venom is proteolytic.
Tarantulas
Tarantulas, found in the family Theraphosidae, have relatively harmless bites, but they can disperse urticating hairs from their abdomens resulting in local skin reactions, ocular problems, and allergic rhinitis.
There are over 34,000 named species of spiders in the world. Almost all species are venomous, but only a few dozen can harm humans. Most spiders either do not have an adequate amount of venom to cause harm, the venom is not toxic to humans, or the fangs cannot penetrate human skin. Of the few spiders that are of medical importance, envenomation can cause a range of clinical manifestations from skin lesions to systemic illness and even death. Tarantulas have venom but usually cause illness from their urticating hairs.
Spiders with cytotoxic venoms cause local tissue injury. The bite is often painless at first, and then symptoms of pain and swelling at the bite site develop minutes to hours later. Some lesions resolve spontaneously while others go on to ulcerate and, at times, develop significant necrosis requiring medical attention. The recluse spiders (eg, Loxosceles reclusa and Loxosceles laeta) have cytotoxic venoms.
Bites from spiders with neurotoxic venoms affect the neuromuscular junctions, causing systemic symptoms from cholinergic and catecholamine excess. Often, the bite is very painful, and systemic symptoms include hypertension, tachycardia, palpitations, diaphoresis, anxiety, shortness of breath, hyperthermia or hypothermia, excessive salivation, nausea, vomiting, and severe pain. The widow spiders, Latrodectus species, have neurotoxic venoms.
The severity of a spider bite depends on the type and amount of venom injected, the site of the bite, and the health and age of the patient. Classically, spider bites are asymptomatic in children. However, when symptomatic (because of the large quantity of venom per kilogram), children are more likely to have systemic reactions than adults.
While there are no spiders that can be described as "truly deadly" (ie, lack of treatment can be expected to result in death), spiders of medical importance include:
Widow spiders
Spiders of the Latrodectus genus are found worldwide and have neurotoxic venoms, with alpha-latrotoxin as the major component that can cause severe systemic symptoms from massive neurotransmitter release. The bite is sharp and painful, and fang marks, diaphoresis, and a halo-like lesion may be seen.
In children, most black widow spider bites become asymptomatic within 48 hours. In more severe black widow bites, however, children can also experience diaphoresis, emesis, and abdominal pain. The abdominal pain can often be confused with peritonitis, and thus a careful history is necessary. Of note, those with peritonitis have pain with movement, while those with a spider bite are hypertensive and agitated, and move frequently to find a comfortable position.
Special Considerations in Infants:
Infants bitten by black widow spiders may present differently from toddlers or children, with non-specific signs and symptoms including poor feeding, irritability, and occasionally full body erythema. Often there is a history of sleeping in a bed that was stored in an outdoor shed.
False black widow spiders
Steatoda spiders are found worldwide and have venom capable of producing symptoms similar to Latrodectus but milder.
Recluse spiders
Spiders of the Loxosceles genus are found worldwide in temperate and tropical regions. Envenomation can cause local necrosis and, rarely, severe systemic symptoms. The brown recluse spider is regularly and erroneously blamed as the cause of necrotic lesions throughout the United States, although this spider is only endemic to the southeastern states.
In severe cases of Loxosceles envenomation in children, patients may present with hemolytic anemia, rhabdomyolysis, acute renal failure, or cellulitis. The most common admission diagnoses for spider bites include hemolytic anemia, cellulitis, and acute renal failure.
Hobo spiders
In the Pacific Northwest, the hobo spider (Tegenaria agrestis) is often blamed as the cause of necrotic skin lesions. However, there is only one documented case of hobo spider envenomation causing dermonecrosis. Other presumed cases are based on anecdotal reports and circumstantial evidence.
Yellow sac spiders
Yellow sac spiders, Cheiracanthium species, are found in North America, Europe, Africa, Asia, Australia, and the Pacific Islands. Envenomation is believed to cause dermonecrosis, but like the hobo spider, T. agrestis, and wolf spider, Lycosa species, the data do not support this association.
Wolf spiders
The wolf spiders, Lycosa species, are common spiders found worldwide. The bite from a wolf spider is typically transiently painful, generally lasting only several minutes. A local reaction might be evident; systemic symptoms are rare. There are no data to support the belief that envenomation causes necrotic lesions.
Banana spiders
Phoneutria species, of Central and South America, have extremely potent venom that is neurotoxic and can be lethal.
Australian funnel-web spiders
Atrax/Hadronyche species in Australia include the most dangerous spider, the Sydney funnel-web spider (Atrax robustus). The venom of this spider is neurotoxic, capable of producing severe pain at the bite site and systemic symptoms that can, rarely, be fatal within minutes.
Six-eyed crab spiders
Spiders of the Sicarius genus are found in Africa and South America and are considered to be extremely venomous but, fortunately, live in remote areas. Their venom is proteolytic.
Tarantulas
Tarantulas, found in the family Theraphosidae, have relatively harmless bites, but they can disperse urticating hairs from their abdomens resulting in local skin reactions, ocular problems, and allergic rhinitis.
Codes
ICD10CM:
T63.391A – Toxic effect of venom of other spider, accidental, initial encounter
SNOMEDCT:
403149008 – Spider bite wound
T63.391A – Toxic effect of venom of other spider, accidental, initial encounter
SNOMEDCT:
403149008 – Spider bite wound
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/15/2016
Last Updated:11/15/2016
Last Updated:11/15/2016
 Patient Information for Spider bite in Child
Patient Information for Spider bite in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Spider bite in Child