Potentially life-threatening emergency
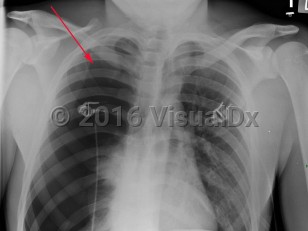
Spontaneous pneumothorax
See also in: PulmonaryAlerts and Notices
Important News & Links
Synopsis

Spontaneous pneumothorax (SP) is caused by the introduction of air between the visceral and parietal pleura, typically as the result of trauma. SP can be classified as either primary or secondary. The presence or absence of lung disease distinguishes the primary form from the secondary form. Primary SP (PSP) lacks underlying lung disease, whereas secondary SP (SSP) patients have a preexisting condition such as chronic obstructive pulmonary disease (COPD; a majority of cases), cystic fibrosis, pulmonary infection, interstitial lung disease (especially histiocytosis and sarcoidosis), AIDS, neoplasms, or drug use.
SP is most often seen in males (6:1 male to female), with tall, thin men being at higher risk. Smoking greatly increases the risk as well (20:1 smokers to nonsmokers). In 20- to 40-year-olds, PSP is usually caused by trauma, whereas those over 40 typically have SSP. In the neonate, SP can be seen in patients with hyaline membrane disease or aspiration. A family history is reported in 11% of patients.
The size of the pneumothorax, rate of development, and underlying clinical status determine the clinical presentation. Those with a mild PSP may not seek care, while those with SSP present acutely. The range of signs and symptoms include acute pleuritic chest pain (localized to the side of the pneumothorax), dyspnea, decreased breath sounds, tachypnea, tachycardia, hyperresonance, unilaterally decreased lung sounds, or acute decompensation.
Tension pneumothorax (TP), while rare, may result from an SP. TP, a life-threatening condition, is caused by pressurized air in the pleural space that displaces mediastinal structures and compromises cardiopulmonary function.
Related topic: Pneumothorax
SP is most often seen in males (6:1 male to female), with tall, thin men being at higher risk. Smoking greatly increases the risk as well (20:1 smokers to nonsmokers). In 20- to 40-year-olds, PSP is usually caused by trauma, whereas those over 40 typically have SSP. In the neonate, SP can be seen in patients with hyaline membrane disease or aspiration. A family history is reported in 11% of patients.
The size of the pneumothorax, rate of development, and underlying clinical status determine the clinical presentation. Those with a mild PSP may not seek care, while those with SSP present acutely. The range of signs and symptoms include acute pleuritic chest pain (localized to the side of the pneumothorax), dyspnea, decreased breath sounds, tachypnea, tachycardia, hyperresonance, unilaterally decreased lung sounds, or acute decompensation.
Tension pneumothorax (TP), while rare, may result from an SP. TP, a life-threatening condition, is caused by pressurized air in the pleural space that displaces mediastinal structures and compromises cardiopulmonary function.
Related topic: Pneumothorax
Codes
ICD10CM:
J93.11 – Primary spontaneous pneumothorax
SNOMEDCT:
80423007 – Spontaneous Pneumothorax
J93.11 – Primary spontaneous pneumothorax
SNOMEDCT:
80423007 – Spontaneous Pneumothorax
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/24/2017
Last Updated:08/24/2017
Last Updated:08/24/2017
Potentially life-threatening emergency
Spontaneous pneumothorax
See also in: Pulmonary