SSSS is mainly a disease of infants and children younger than 6, with a higher incidence seen in males. With appropriate antibiotics, SSSS often resolves entirely in 1-2 weeks. However, many adults who suffer from SSSS have underlying medical problems such as renal insufficiency, and mortality rates are estimated at 60% or higher in immunocompromised patients.
In the United States, phage group II staphylococci are the most common toxin-producing strains. These phage group II strains can be methicillin-sensitive and resistant and produce exotoxins (epidermolytic toxins A and B or ETA and ETB, respectively) that cause intraepidermal cleavage with subsequent superficial sloughing. Specifically, ETA and ETB are serine proteases that cleave the extracellular domain of desmoglein 1, a molecule that facilitates keratinocyte adhesion. Note that bullous impetigo and toxic shock syndrome are also toxin-mediated diseases considered within the same spectrum of SSSS.
The natural history of SSSS is characterized by the following:
- Prodromal symptoms and/or purulent rhinorrhea and/or conjunctivitis
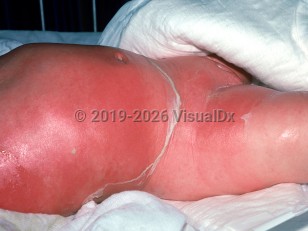
- Facial erythema that generalizes to the body in less than 48 hours
- Bullae development, positive Nikolsky's sign, and very tender skin
- Skin wrinkling and epidermal sloughing within 48 hours after bullae develop
- Desquamation continues for up to 5 days
- Re-epithelialization without scarring in approximately 2 weeks