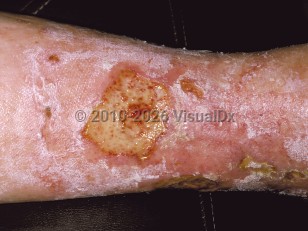
Stasis ulcer
Alerts and Notices
Important News & Links
Synopsis

Stasis ulcers, or venous ulcers, are ulcers due to venous insufficiency. They are large, irregularly shaped, shallow ulcers that often demonstrate a yellow exudate covering the wound bed. They are most commonly found in the medial malleolar region of the lower extremity. While the reported prevalence varies, it is estimated that approximately 0.05%-1.52% of Americans suffer from venous ulcers. An increased prevalence is seen with age, and both sexes are affected equally. Additional risk factors include a history of thrombosis, phlebitis, leg injury such as fracture or trauma, pregnancy, obesity, lower socioeconomic status, and social isolation.
The primary pathophysiology involves incompetent one-way venous valves or dysfunctional calf muscle pumping, leading to insufficient venous blood return to the heart and chronic leg venous hypertension. This venous hypertension leads to aberrant tissue perfusion and subsequent decreased delivery of oxygen and nutrients, failure to remove metabolic byproducts, and tissue ischemia.
Additional clinical features commonly associated include leg and ankle edema, varicose veins, yellow-brown pigmentation secondary to hemosiderin deposition and extravasated red blood cells, eczematous changes with scaling and crusting (stasis dermatitis), and lymphedema. Lipodermatosclerosis is also seen and corresponds to fibrotic changes in subcutaneous tissue leading to a hard and indurated feel to the skin. An "inverted champagne bottle" leg indicates end stage lipodermatosclerosis and is caused by severe fibrotic changes in the distal leg and leg edema of the proximal leg. Atrophie blanche are smooth, ivory-colored atrophic plaques secondary to sclerosis seen in approximately 40% of patients with venous insufficiency.
Additional key points are that stasis ulcers usually begin on the medial malleolus but may become circumferential over time. They may be painful, are difficult to treat, and frequently recur. They may become secondarily infected.
The primary pathophysiology involves incompetent one-way venous valves or dysfunctional calf muscle pumping, leading to insufficient venous blood return to the heart and chronic leg venous hypertension. This venous hypertension leads to aberrant tissue perfusion and subsequent decreased delivery of oxygen and nutrients, failure to remove metabolic byproducts, and tissue ischemia.
Additional clinical features commonly associated include leg and ankle edema, varicose veins, yellow-brown pigmentation secondary to hemosiderin deposition and extravasated red blood cells, eczematous changes with scaling and crusting (stasis dermatitis), and lymphedema. Lipodermatosclerosis is also seen and corresponds to fibrotic changes in subcutaneous tissue leading to a hard and indurated feel to the skin. An "inverted champagne bottle" leg indicates end stage lipodermatosclerosis and is caused by severe fibrotic changes in the distal leg and leg edema of the proximal leg. Atrophie blanche are smooth, ivory-colored atrophic plaques secondary to sclerosis seen in approximately 40% of patients with venous insufficiency.
Additional key points are that stasis ulcers usually begin on the medial malleolus but may become circumferential over time. They may be painful, are difficult to treat, and frequently recur. They may become secondarily infected.
Codes
ICD10CM:
I83.009 – Varicose veins of unspecified lower extremity with ulcer of unspecified site
SNOMEDCT:
41915009 – Stasis ulcer
I83.009 – Varicose veins of unspecified lower extremity with ulcer of unspecified site
SNOMEDCT:
41915009 – Stasis ulcer
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/11/2018
Last Updated:02/12/2019
Last Updated:02/12/2019
 Patient Information for Stasis ulcer
Patient Information for Stasis ulcer
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Stasis ulcer