SJS/TEN spectrum drug hypersensitivity:
- Induced strictly by medication exposure (sulfamethoxazole / trimethoprim, NSAIDs, allopurinol, antiepileptics, etc)
- SJS when less than 10% BSA is involved, SJS/TEN overlap when 10%-30% BSA is involved, TEN when greater than 30% BSA is involved
- Dusky macules (so-called "targetoid" with 2 zones of color) evolving into flaccid bullae and skin desquamation
- Skin lesions favor truncal sites
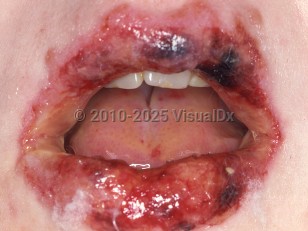
- Oral, ocular, and genitourinary mucositis
- Nikolsky sign and Asboe-Hansen sign are positive (see descriptions in Look For)
- Skin pain as a sign alerting to this diagnosis
- Secondary to infection, typically herpes simplex virus (HSV), or medication
- Presents with typical, true target lesions (3 zones of color as opposed to 2 zones of color in SJS/TEN)
- Lesions predominate on acral locations, particularly palms and soles
- Lesions may or may not be vesiculated but do not desquamate or result in widespread erosions as seen in SJS/TEN
- Mucositis may be entirely absent or limited to a single mucosal site and skin findings are more prominent than mucositis
- Nikolsky sign is negative
- Secondary to Mycoplasma or other infection as evidenced by clinical pneumonia, imaging studies, and/or Mycoplasma titers
- Pronounced oral and ocular mucositis with absent, spare, or mild cutaneous involvement
- Cutaneous lesions are most often tense and vesiculobullous, with or without target or targetoid lesions
- Cutaneous lesions do not erode or desquamate as seen in SJS/TEN (Note: erosion is seen in the genital and perianal skin, which are considered akin to mucosal surfaces)
- Nikolsky sign is negative
In SJS/TEN, common drug precipitants include sulfonamides, phenytoin, lamotrigine and other anticonvulsants, allopurinol, penicillins, and NSAIDs. Studies have linked certain HLA haplotypes and genetic p450 polymorphisms to increased risk of SJS/TEN when exposed to specific medications. AIDS is associated with a thousandfold increased risk of SJS/TEN.
More commonly in children, infections rather than drugs are pointed out as the main precipitant of SJS/TEN. This contributes in part to the higher rate of SJS/TEN recurrence in children, given that many infections can recur and cannot be as easily avoided as foregoing a particular drug.
All reported cases in infants younger than 6 months have been due to either bacterial sepsis combined with multiple antibiotic regimens or acute graft-versus-host disease (GVHD). In infants and neonates, SJS/TEN is exceedingly rare. Cases were often associated with gram-negative bacteremia and lack confirmatory histopathology. Consideration of more common diagnoses should be carefully evaluated.
SJS/TEN runs an unpredictable clinical course. It is typically preceded by nonspecific prodromal symptoms followed by characteristic skin and mucosal lesions.
Prodromal symptoms include fevers, malaise, arthralgias / myalgias, ocular irritation, upper respiratory tract symptoms, and oropharyngeal pain and may precede skin / mucosal findings by 1-3 days. Importantly, cutaneous pain or burning skin is a prominent early feature of SJS/TEN, and its presence could signify an ominous sign of impending necrolysis.
Cutaneous lesions may begin as a more typical exanthematous eruption that evolves to dusky, irregular, ill-defined coalescing macules with purpuric or detached centers. Lesions typically appear first on the central trunk, palms, and soles and then spread to involve the face and proximal extremities. As the disease progresses, large areas of serous blistering and sloughing may occur. Skin is typically painful and tender.
Mucosal lesions: Oral mucosal sloughing and crusting are present in more than 90% of cases, and ocular involvement is present in more than 80%. Urogenital and, more rarely, respiratory and gastrointestinal (GI) mucosa may also be involved.
With severe involvement of the eyes, ulceration, scarring, visual impairment, and ultimately blindness may result. An estimated 50%-90% of patients will experience chronic ocular sequelae that may develop as long as 8 years following acute SJS/TEN.
Esophageal, anal, vaginal, and urethral meatal stenosis may be seen. GI bleeding, hepatitis, urinary retention, nephritis, anuria from dehydration and genitourinary injury, myocarditis, pneumothorax, obtundation, and seizures are rare complications. Other involvement includes GI lesions with diarrhea, cystitis, splenic inflammation, arthritis, pneumonitis, otitis media, paronychia, and nail shedding.
Prognosis: SJS carries a 1%-5% mortality risk, may or may not have systemic symptoms, and involves the trunk and face with many isolated lesions. TEN carries a 25%-35% mortality risk and invariably has systemic symptoms, and the lesions on the trunk and face are largely coalesced. Secondary infection of denuded skin plays a significant role in mortality, as does respiratory compromise from mucositis.
Risk factors that confer a worse prognosis include extent of BSA involved, underlying malignancy, number of medications, leukopenias, and elevated serum urea, glucose, and creatinine levels. SCORTEN is a prognostic scoring system for patients with epidermal necrolysis that contemplates many of the above-mentioned risk factors and several others. While SCORTEN was validated in adults, studies have demonstrated that other pediatric-tailored assessment tools are not superior to SCORTEN in children, which has accurately predicted clinical outcomes.
Rapid identification and withdrawal of the offending drug and transfer to a burn unit with aggressive supportive care are the most critical steps in management. Fortunately, SJS/TEN mortality seems to be lower in children when compared to adults. It is of utmost importance to closely follow, manage, and strive to mitigate the potential long-term ocular and genitourinary complications.
Related topic: postacute sequelae of SJS and TEN