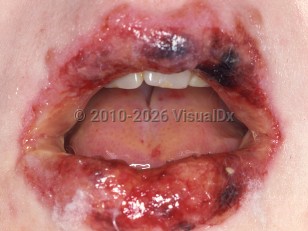
Stevens-Johnson syndrome - External and Internal Eye
See also in: Overview,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

SJS has been defined as involvement of detached and detachable skin that is less than 10% of body surface area (BSA), while TEN involves greater than 30% BSA. SJS-TEN overlap occurs when 10%-30% BSA is involved. However, the newer Niigata criteria define TEN as involvement of 10% BSA or greater. Note that SJS can rapidly evolve into TEN, and both can have an unpredictable clinical course.
Investigations over the past decade have provided strong evidence that SJS and TEN are secondary to the host's inability to detoxify the culprit drug and its metabolites. This results in a cell-mediated immune response that activates cytotoxic T-cells and induces keratinocyte apoptosis via cell surface death receptor signaling. The primary medications most frequently implicated include allopurinol, NSAIDs, antibiotics, and anticonvulsants. Additional causes, albeit rare, include immunizations and infections.
Photodistributed SJS/TEN is a rarely reported phenomenon. Almost all reported patients have been women on an antibiotic, an anticonvulsant, or NSAID therapy who developed SJS/TEN limited to photoexposed areas 24-72 hours after sun or tanning bed exposure. Sun-covered mucosal surfaces were also affected.
SJS/TEN can affect all ages and races, with a slight preponderance seen in women (1.5:1) and an increasing incidence with age. Studies have linked certain HLA haplotypes and genetic p450 polymorphisms to increased risk of SJS/TEN when exposed to specific medications. AIDS is associated with a thousandfold increased risk of SJS/TEN.
The onset of SJS/TEN occurs 1-3 weeks, and sometimes as long as 8 weeks, after the ingestion of the culprit medication. It is typically preceded by nonspecific prodromal symptoms followed by characteristic skin and mucosal lesions.
Prodromal symptoms include fevers, malaise, arthralgias / myalgias, ocular irritation, upper respiratory tract symptoms, and oropharyngeal pain and may precede skin / mucosal findings by 1-3 days. Importantly, cutaneous pain or burning skin is a prominent early feature of SJS/TEN, and its presence could signify an ominous sign of impending necrolysis.
Cutaneous lesions may begin as a more typical exanthematous eruption that evolves to dusky, irregular, ill-defined coalescing macules with purpuric or detached centers. Lesions typically appear first on the central trunk, palms, and soles and then spread to involve the face and proximal extremities. As the disease progresses, large areas of serous blistering and sloughing may occur. Skin is typically painful and tender.
Mucosal lesions: Oral mucosal sloughing and crusting is present in more than 90% of cases and ocular involvement in more than 80%. Urogenital and, more rarely, respiratory and gastrointestinal (GI) mucosa may also be involved.
With severe involvement of the eyes, ulceration, scarring, visual impairment, and ultimately blindness may result. An estimated 50%-90% of patients will experience chronic ocular sequelae that may develop as long as 8 years following acute SJS/TEN.
Esophageal, anal, vaginal, and urethral meatal stenosis may be seen. GI bleeding, hepatitis, urinary retention, nephritis, anuria from dehydration and genitourinary injury, myocarditis, pneumothorax, obtundation, and seizures are rare complications. Other involvement includes GI lesions with diarrhea, cystitis, splenic inflammation, arthritis, pneumonitis, otitis media, paronychia, and nail shedding.
Prognosis: SJS carries a 1%-5% mortality risk, may or may not have systemic symptoms, and involves the trunk and face with many isolated lesions. TEN carries a 25%-35% mortality risk, invariably has systemic symptoms, and the lesions on the trunk and face are largely coalesced. Secondary infection of denuded skin plays a significant role in mortality, as does respiratory compromise from mucositis.
Risk factors that confer a worse prognosis include extent of BSA involved, older age, malignancy, number of medications, leukopenias, and elevated serum urea, glucose, and creatinine levels. SCORTEN is a prognostic scoring system for patients with epidermal necrolysis that contemplates many of the above-mentioned risk factors and several others.
Rapid identification and withdrawal of the offending drug and transfer to a burn unit with aggressive supportive care are the most critical steps in management.
Long-term ocular and genitourinary follow-up is vital in mitigating complications.
Related topic: postacute sequelae of SJS and TEN
Codes
L51.1 – Stevens-Johnson syndrome
SNOMEDCT:
73442001 – Stevens-Johnson syndrome
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:01/22/2025